What does fact checked mean?
At Healthfully, we strive to deliver objective content that is accurate and up-to-date. Our team periodically reviews articles in order to ensure content quality. The sources cited below consist of evidence from peer-reviewed journals, prominent medical organizations, academic associations, and government data.
The information contained on this site is for informational purposes only, and should not be used as a substitute for the advice of a professional health care provider. Please check with the appropriate physician regarding health questions and concerns. Although we strive to deliver accurate and up-to-date information, no guarantee to that effect is made.
How to Lose 40 Pounds in 4 to 6 Weeks
Being fit and healthy is quite a challenge in today's fast-paced world. Weight loss should be treated as a change of lifestyle, not just a short-term change of eating habits 3. You can loose 40 pounds in a little over a month if you follow some basic steps rigorously, but you should keep eating healthy and exercising even after you achieve your goal, or you run a risk of gaining it all back.
Add nonstarchy vegetables to your diet. Nonstarchy vegetables are all vegetables apart from peas, corn, potatoes, squash and yams 1. They have a lot of fiber, have low sugar and calorie levels, and are mostly built out of water. All in all, they are the ultimate diet food.
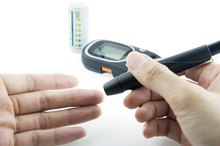
How to Get Sugar Out of Your Body
Learn More
Stop eating at least three hours before you go to sleep at night. When you sleep, you don't use much energy, and your metabolism slows down. Your body will store the majority of whatever you eat in the evening as fat. This is a very bad eating habit.
Cut sugar out of your diet. Sugar gives you the feeling of being full for a very short time, and when the sugar levels in your blood drop you will feel hunger again. Sugar that you don't burn off goes directly to your fat cells. If you need a kick of sugar after your meal, try a bar of black chocolate. For four to six weeks you should stay away from all sugar, including fruit and dried fruit.
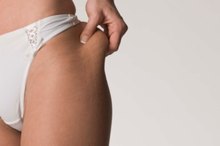
What Not to Eat to Lose Thigh Weight?
Learn More
Make exercising a part of your routine. Pick something that is at least mildly entertaining for you, but try to find a combination between cardio exercise and weights. Do it at least three times per week, but ideally you should work out five times for an hour every week.
Keep your meals small and eat six to eight times a day. This trick will make your stomach smaller, which will enable you to eat smaller portions, and sustain your blood sugar levels, so there will be no drastic ups and downs, which result in your craving bad foods.
Eat a lot of things that keep you feel full for a long time, such as meat, fish, and wholegrain carbs. Don't eat things that are white, such as white sugar, pasta, white bread, etc. which are usually the foods your body devours quickly. Replace them with their dark or wholegrain alternatives.
Drink only water. Juices and fizzy drinks have a lot of sugar in them. If you are a tea or coffee person, put nonfat milk in them and drink them without sugar. For motivation, calculate how much sugar you eat only with your cups of coffee every day.
Related Articles
References
- Vegetables and weight loss
- Eating before sleeping is never recommended
- Sugar and weight loss
- What does it take to lose weight?
- Giugliano D, Maiorino MI, Bellastella G, Esposito K. More sugar? No, thank you! The elusive nature of low carbohydrate diets. Endocrine. 2018;61(3):383-387. doi:10.1007/s12020-018-1580-x
- DiNicolantonio JJ, Lucan SC, O'Keefe JH. The evidence for saturated fat and for sugar related to coronary heart disease. Prog Cardiovasc Dis. 2016;58(5):464-472. doi:10.1016/j.pcad.2015.11.006
- Stanhope KL. Sugar consumption, metabolic disease and obesity: the state of the controversy. Crit Rev Clin Lab Sci. 2016;53(1):52-67. doi:10.3109/10408363.2015.1084990
- Khan TA, Sievenpiper JL. Controversies about sugars: results from systematic reviews and meta-analyses on obesity, cardiometabolic disease and diabetes. Eur J Nutr. 2016;55(Suppl 2):25-43. doi:10.1007/s00394-016-1345-3
- American Heart Association. The facts on fats: 50 years of American Heart Association dietary fats recommendations. Updated June 2015.
- La Berge AF. How the ideology of low fat conquered America. J Hist Med Allied Sci. 2008;63(2):139-77. doi:10.1093/jhmas/jrn001
- Kuzma JN, Schmidt KA, Kratz M. Prevention of metabolic diseases: fruits (including fruit sugars) vs. vegetables. Curr Opin Clin Nutr Metab Care. 2017;20(4):286–293. doi:10.1097/MCO.0000000000000378
- Clemente A, Olias R. Beneficial effects of legumes in gut health. Curr Opin Food Sci. 2017;14:32-36. doi:10.1016/j.cofs.2017.01.005
- U.S. National Library of Medicine, MedlinePlus. Omega-3 fats - Good for your heart. Updated January 13, 2020.
- Westerterp-Plantenga MS, Lemmens SG, Westerterp KR. Dietary protein - its role in satiety, energetics, weight loss and health. Br J Nutr. 2012;108 Suppl 2:S105–S112. doi:10.1017/S0007114512002589
- Choudhury H, Pandey M, Hua CK, et al. An update on natural compounds in the remedy of diabetes mellitus: a systematic review. J Tradit Complement Med. 2017;8(3):361–376. doi:10.1016/j.jtcme.2017.08.012
- University of California, San Francisco, Diabetes Education Online. Diabetes and alcohol.
- Satija A, Bhupathiraju SN, Rimm EB, et al. Plant-based dietary patterns and incidence of type 2 diabetes in US men and women: results from three prospective cohort studies. PLoS Med. 2016;13(6):e1002039. doi:10.1371/journal.pmed.1002039
- United States Department of Agriculture, ChooseMyPlate. Choose a food group to explore.
- U.S. Department of Health and Human Services, U.S. Department of Agriculture. 2015–2020 Dietary Guidelines for Americans. 8th ed. December 2015.
- Kastorini CM, Milionis HJ, Esposito K, Giugliano D, Goudevenos JA, Panagiotakos DB. The effect of Mediterranean diet on metabolic syndrome and its components: a meta-analysis of 50 studies and 534,906 individuals. J Am Coll Cardiol. 2011;57(11):1299–1313. doi:10.1016/j.jacc.2010.09.073
- Welsh JA, Sharma A, Abramson JL, Vaccarino V, Gillespie C, Vos MB. Caloric sweetener consumption and dyslipidemia among US adults. JAMA. 2010;303(15):1490-1497. doi:10.1001/jama.2010.449
Writer Bio
Lucy Natek started writing in 2004. Her work has appeared in publications such as "Sketchbook," "Kismet," "In*tandem" and "Rahha" and on websites such as Dia, Fashion Students Online and Haus Digital. Natek holds a master's degree in political science and international relations from the University of Ljubljana.