What Are the Dangers of Donating Blood Plasma?
Your blood consists of red and white blood cells, platelets and protein-rich liquid called plasma. Donated plasma is used to treat a variety of medical conditions, including burns, blood clotting deficiencies and immunodeficiency disorders. Plasma donation involves withdrawing whole blood, which passes through a machine that harvests the plasma. The blood cells and platelets are then returned to the donor. Plasma donation is generally safe for healthy adults who meet donor eligibility requirements. However, side effects can occur. Most are minor and do not pose a significant health threat. Serious side effects are very rare but possible.
Bruising and Nerve Irritation
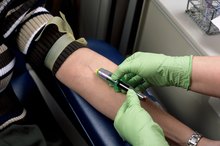
Bruising or discomfort at the site of needle insertion is the most common side effect of plasma donation. This occurs in less than 2 percent of donations, according to a large study published in 2013 in the "Asian Journal of Transfusion Science." Bruising is typically mild, posing no health threat other than minor discomfort and possible swelling. Recommended treatment includes periodic application of a cold compress for the first 12 to 24 hours, followed by warm compresses until the bruise resolves or no longer causes discomfort.
Rarely, insertion of the donation needle causes nerve irritation. When this occurs, it typically triggers immediate, intense pain at the insertion site. Shooting pain often extends down the arm and possibly into the hand. Should this occur, the needle is immediately removed and the donation typically deferred until another day. Removal of the needle typically eliminates the pain, although there might be some mild, temporary residual discomfort.
- Bruising or discomfort at the site of needle insertion is the most common side effect of plasma donation.
- Recommended treatment includes periodic application of a cold compress for the first 12 to 24 hours, followed by warm compresses until the bruise resolves or no longer causes discomfort.
Lightheadedness and Fainting
Venipuncture Complications
Learn More
Plasma and other types of blood donation sometimes provoke an involuntary reflex call a vagovagal response, which leads to a decrease in blood pressure. The sight of blood or the collection needle, pain from the needle insertion, or anxiousness about the donation process can trigger this reaction. Early symptoms might include:
- sweating
- sudden warmness
- weakness
- paleness
- nausea or vomiting
- blurry or tunnel vision,
- dizziness
These symptoms might quickly progress to fainting, but can often be averted with immediate intervention -- such as reclining the donation chair so that the feet are raised and applying a cool compress to the forehead. If fainting or vomiting occurs, the donation is immediately discontinued.
- Plasma and other types of blood donation sometimes provoke an involuntary reflex call a vagovagal response, which leads to a decrease in blood pressure.
- The sight of blood or the collection needle, pain from the needle insertion, or anxiousness about the donation process can trigger this reaction.
Citrate Reaction
When donating plasma, a chemical called citrate is added to the blood as it enters the separating machine to prevent clotting. Most of the citrate remains in the donated plasma, but some enters the bloodstream when the blood cells are returned to the donor's circulation. Citrate temporarily binds charged calcium molecules in the body. Due to the small proportion of calcium bound and the rapid rate of citrate metabolism, citrate usually causes no side effects. However, roughly 1 percent of plasma donations lead to a citrate reaction. Most reactions are mild and include symptoms such as tingling or a vibratory sensation around the mouth, in the face, or in the hands or feet; cramps in the hands or feet; and weakness or lack of energy.
With a mild citrate reaction, the donation process is usually paused. Taking oral calcium tablets and lowering the rate of citrate entering the bloodstream often suffices to eliminate these side effects. With a severe citrate reaction, the donation is immediately discontinued. Depending on the severity of the symptoms, emergency medical care may be needed, although this is very rare.
- When donating plasma, a chemical called citrate is added to the blood as it enters the separating machine to prevent clotting.
- Taking oral calcium tablets and lowering the rate of citrate entering the bloodstream often suffices to eliminate these side effects.
Other Possible Risks
Disadvantages to Donating Plasma
Learn More
The needle for plasma donation is placed in an arm vein. Rarely, the needle might be inserted into an artery instead of a vein. Because of the higher pressure in arteries, this might lead to bleeding into the arm tissues around the site of the arterial puncture. Should the needle enter an artery, it is immediately removed and firm pressure held on the site for at least 10 minutes. Continued bleeding from a punctured artery requires urgent medical care, but this is rare.
Other possible but rare complications that might occur with plasma donation include: -- infection at the site of the needle insertion -- formation of a blood clot in the vein used for the donation -- irritation, itchiness or hives at the donation site -- blood loss if the donation is halted before returning the blood cells to the donor
- The needle for plasma donation is placed in an arm vein.
- Because of the higher pressure in arteries, this might lead to bleeding into the arm tissues around the site of the arterial puncture.
Considerations, Warnings and Precautions
Many plasma donors find the process a rewarding way to share their good health with other who are less fortunate. Plasma donation is generally safe and poses a low risk for serious complications when performed by appropriately trained and licensed medical professionals who comply with all relevant U.S. Food and Drug Administration regulations for plasma collection facilities 2.
Whether you're a first-time or regular plasma donor, it's important to follow all preparatory and followup instructions. At each visit, you will be evaluated to determine whether you are eligible to donate. It is critically important to answer all eligibility screening questions honestly -- for your safety and the safety of people who might receive your plasma.
If you develop any new signs or symptoms after donating plasma, contact the donation center right away. Seek immediate medical attention if you experience shortness of breath, fainting, chest pain or other symptoms that concern you.
Reviewed and revised by: Tina M. St. John, M.D.
- Many plasma donors find the process a rewarding way to share their good health with other who are less fortunate.
- At each visit, you will be evaluated to determine whether you are eligible to donate.
Related Articles
References
- Asian Journal of Transfusion Science: Adverse Events Associated With Apheresis Procedures: Incidence and Relative Frequency
- U.S. Food and Drug Administration: Code of Federal Regulations Title 21
- Plasma Protein Therapeutics Association: Citrate Anticoagulant and Apheresis -- Perspective of Plasma Protein Therapeutics Industry
- The United Network For Organ Sharing
- Transplant Living, a Division of UNOS. TransplantLiving.org
Writer Bio
Jonathan Croswell has spent more than five years writing and editing for a number of newspapers and online publications, including the "Omaha World-Herald" and "New York Newsday." Croswell received a Bachelor of Arts degree in English from the University of Nebraska and is currently pursuing a Master's of Health and Exercise Science at Portland State University.