Normal Oxygen Saturation for Infants
The health of an infant is assessed in various ways, including observation and measurement of important blood components. Measurement of oxygen saturation provides information about a child's respiratory, heart and circulatory health. It is part of an assessment of vital signs for an infant, particularly if the newborn is premature or experiences breathing difficulty.
Oxygen Saturation
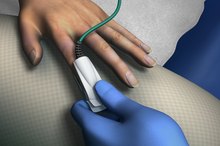
Oxygen saturation reflects the quantity of hemoglobin in the blood that is saturated with oxygen. Hemoglobin is the component of red blood cells that binds oxygen and transports it to body tissues. Oxygen saturation is commonly measured by pulse oximetry 1. This instrument uses an infrared light source to detect oxygen saturation without collecting a blood sample. A pulse oximeter is typically wrapped around an infant’s foot or hand to obtain a measurement.
- Oxygen saturation reflects the quantity of hemoglobin in the blood that is saturated with oxygen.
- This instrument uses an infrared light source to detect oxygen saturation without collecting a blood sample.
Full-Term Infants
Why Oxygen With CPAP?
Learn More
A healthy, full-term baby should have an oxygen saturation of 95 to 100 percent. Some health care facilities may have slightly different parameters. Full-term newborns who require supplemental oxygen after birth may have slightly lower oxygen saturation levels.
Premature Infants
Babies born prematurely have lower oxygen saturation levels initially because their lungs are not fully developed. Normal oxygen saturation for a preterm infant is roughly 84 to 90 percent. A newborn who is unable to maintain a minimum oxygen saturation level -- whether full-term or premature -- may be placed on supplemental oxygen. The health care team monitors an infant's oxygen saturation level and adjusts the flow rate and concentration of supplemental oxygen to maintain a normal level.
- Babies born prematurely have lower oxygen saturation levels initially because their lungs are not fully developed.
Hypoxemia
Infant Blood Sugar Levels
Learn More
Infants with an oxygen saturation level below a normal level have hypoxemia -- or oxygen deficiency. For an infant not wearing a pulse oximeter, hypoxemia may not be readily apparent. For example, a bluish discoloration around the lips called cyanosis is a physical sign of low blood oxygen. However, this sign often does not develop until the oxygen saturation drops to 75 percent or less in a full-term infant.
- Infants with an oxygen saturation level below a normal level have hypoxemia -- or oxygen deficiency.
Retinopathy of Prematurity
Maintaining a lower oxygen saturation than typically considered normal may be acceptable or preferable in some situations. Because lung tissue is one of the last to fully develop in a fetus, premature babies frequently require supplemental oxygen. Treatment with high levels of oxygen may lead to retinopathy of prematurity, an eye disorder that can lead to blindness. Adjusting the supplemental oxygen to maintain oxygen saturation at a lower level decreases the occurrence of ROP.
- Maintaining a lower oxygen saturation than typically considered normal may be acceptable or preferable in some situations.
- Because lung tissue is one of the last to fully develop in a fetus, premature babies frequently require supplemental oxygen.
Related Articles
References
- American Association of Critical Care Nurses: Oxygen Saturation Monitoring by Pulse Oximetry
- Children’s National Medical Center: Congenital Heart Disease Screening - Frequently Asked Questions
- University of Michigan Department of Pediatrics: Maintaining Saturations Between 70-90% in Preterm Infants Reduces the Incidence of Retinopathy of Prematurity
- Lippincott's Nursing Center: Hypoxemia in the Term Newborn
- McGill University, Office for Science and Society, "Under the Microscope: Blood"
- Collins JA, Rudenski A, Gibson J, Howard L, O'Driscoll R. Relating oxygen partial pressure, saturation and content: the haemoglobin-oxygen dissociation curve. Breathe (Sheff). 2015;11(3):194–201. doi: 10.1183/20734735.001415
- Gossman W, Alghoula F, Berim I. Anoxia (Hypoxic Hypoxia) [Updated 2019 Jul 11]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-.
- Giaccia AJ, Simon MC, Johnson R. The biology of hypoxia: the role of oxygen sensing in development, normal function, and disease. Genes Dev. 2004;18(18):2183–2194. doi: 10.1101/gad.1243304
- Leach RM, Treacher DF. Oxygen transport-2. Tissue hypoxia. BMJ. 1998;317(7169):1370–1373. doi: 10.1136/bmj.317.7169.1370
- Hafen BB, Sharma S. Oxygen Saturation. [Updated 2019 Jun 2]. In: StatPearls Treasure Island (FL): StatPearls Publishing. 2019 Jan.
Writer Bio
Meg Brannagan has worked as a registered nurse for more than 10 years, specializing in women's and children's health. She holds a bachelor's degree in nursing from the University of Nebraska Medical Center.