What does fact checked mean?
At Healthfully, we strive to deliver objective content that is accurate and up-to-date. Our team periodically reviews articles in order to ensure content quality. The sources cited below consist of evidence from peer-reviewed journals, prominent medical organizations, academic associations, and government data.
- Khunger N, et al. (2008). Standard guidelines of care for chemical peels.
- Khunger N, et al. (2008). Standard guidelines of care for chemical peels.
- Mayo Clinic Staff. (2018). Chemical peel.
The information contained on this site is for informational purposes only, and should not be used as a substitute for the advice of a professional health care provider. Please check with the appropriate physician regarding health questions and concerns. Although we strive to deliver accurate and up-to-date information, no guarantee to that effect is made.
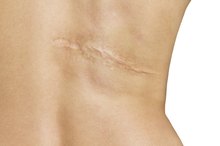
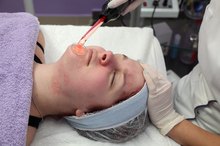
How to Treat a Scar From a TCA Peel
A trichloracetic acid (TCA) peel is considered a medium-level peel designed to penetrate the outer layers of skin. When applied to the skin, the peel burns away damaged and dead layers of skin to reveal fresher skin underneath. After the TCA peel heals, results include reduction in blemishes, age spots and wrinkles, according to DocShop.com. Because a TCA peel causes a crust to form over the skin, it is possible to experience scarring following a chemical peel, according to the American Academy of Dermatology 2.
Apply a scar treatment cream to the area to soften the scar. DERMADoctor suggests using Mederma, which is designed to soften scar tissue and improve the appearance of new scars. Scar treatment creams must be applied several times a day to continually help the scar fade.
Skin Bleach for Scars
Learn More
Place a silicone gel sheeting over the scarred area. Silicone sheeting has been shown to reduce the size and raised appearance of a scar, according to DERMADoctor. This sheeting often resembles a bandage and can stay on the area for a day or more. Examples of silicone gel sheeting include ScarGuard MD and Kelo-cote Scar Gel.
Undergo a treatment, such as microdermabrasion, designed to reduce scars like TCA chemical peel scars 2. Microdermabrasion is a treatment used by dermatologists and aestheticians to reduce a scar’s appearance by removing the top layer of skin that may have scar tissue on it. Other treatment options that may prove more invasive include laser resurfacing and scar removal via a surgical process known as subcision.
Tazorac for Wrinkles
Learn More
Allow time for the scar to heal. It is not uncommon for areas to appear hyperpigmented following a TCA peel. These areas of discoloration can be mistaken for scars, according to the American Academy of Dermatology. However, with time, the pigmentation will even out, reducing redness and any brown spots that may occur.
Tips
A dermatologist should evaluate you for the potential to develop scarring prior to administering a chemical peel. Those who are prone to fever blisters, cold sores or keloids are more likely to develop scars, according to the American Academy of Dermatology.
Avoid the sun while undergoing treatments for scarring following chemical peels. The sun can cause the scar to become darker or lighter than the surrounding skin, making it appear more noticeable.
Related Articles
References
- Anitha B. (2010). Prevention of complications in chemical peeling. DOI:
- Chemical peels: What is a chemical peel?
- Cosmetic surgery national data bank statistics. (2018).
- Dayal S, et al. (2017). Clinical efficacy and safety on combining 20% Trichloroacetic Acid peel with topical 5% ascorbic acid for melasma. DOI:
- Khunger N, et al. (2008). Standard guidelines of care for chemical peels.
- Kumari R, et al. (2010). Comparative study of trichloroacetic acid versus glycolic acid chemical peels in the treatment of melasma. DOI:
- Mayo Clinic Staff. (2018). Chemical peel.
- Nikalji N, et al. (2012). Complications of medium depth and deep chemical peels. DOI:
- Puri N. (2012). Comparative study of 15% TCA peel versus 35% glycolic acid peel for the treatment of melasma. DOI:
- Wang F, Li X, Wang X, Jiang X. Efficacy of topical silicone gel in scar management: A systematic review and meta-analysis of randomised controlled trials. Int Wound J. 2020 Jun;17(3):765-773. doi: 10.1111/iwj.13337
Writer Bio
Rachel Nall began writing in 2003. She is a former managing editor for custom health publications, including physician journals. She has written for The Associated Press and "Jezebel," "Charleston," "Chatter" and "Reach" magazines. Nall is currently pursuing her Bachelor of Science in Nursing at the University of Tennessee.