What does fact checked mean?
At Healthfully, we strive to deliver objective content that is accurate and up-to-date. Our team periodically reviews articles in order to ensure content quality. The sources cited below consist of evidence from peer-reviewed journals, prominent medical organizations, academic associations, and government data.
- National Endocrine and Metabolic Diseases Information Service: Adrenal Insufficiency and Addison’s Disease
- MayoClinic.com: Age Spots (Liver Spots)
The information contained on this site is for informational purposes only, and should not be used as a substitute for the advice of a professional health care provider. Please check with the appropriate physician regarding health questions and concerns. Although we strive to deliver accurate and up-to-date information, no guarantee to that effect is made.
Dark Pigmentation on the Back
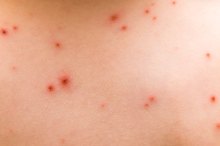
When melanin, the skin's pigment, bunches together in excess to form dark spots on the back, the condition is called hyperpigmentation. Hyperpigmentation itself has a few different common causes, but the options for remedying dark spots are largely the same regardless of the cause. The American Osteopathic College of Dermatology says most cases of dark pigmentation on the back are not a health concern. However, spots on the skin should be examined by a dermatologist to rule out skin cancer.
Causes
Darkened areas of pigmentation on the back are a typical manifestation of long-term exposure to UV radiation from the sun or artificial tanning devices. These areas of dark pigmentation are called solar lentigines, but are more familiarly known as liver, sun or age spots 2. Spots on the back may also be post-inflammatory hyperpigmentation, a generally temporary reaction to inflammation or injury. A disorder called Addison's disease, consisting of underactive adrenal glands, causes hormonal imbalances that may produce areas of dark pigmentation as well.
- Darkened areas of pigmentation on the back are a typical manifestation of long-term exposure to UV radiation from the sun or artificial tanning devices.
- Spots on the back may also be post-inflammatory hyperpigmentation, a generally temporary reaction to inflammation or injury.
Symptoms
Reddish-Brown Spots on the Skin
Learn More
If the areas of pigmentation on your back are solar lentigines, they are flat, clearly delineated, rounded and either brown, black or gray. You may see similar spots on the back of your neck and hands, face, shoulders, forearms or lower legs. There may be other signs of damage from UV radiation, such as wrinkles or a leather-like texture to the skin. If the dark pigmentation on your back is a reaction to inflammation or injury, there may be redness, scabs, scars or other signs of the body's healing process. Addison's disease has many symptoms that generally present gradually, notes the National Endocrine and Metabolic Diseases Information Service. Muscle weakness, fatigue, diminishing appetite, weight loss, digestive upset, mood changes, low blood pressure, low blood sugar, salt cravings, headaches and sweats are other signs and symptoms.
- If the areas of pigmentation on your back are solar lentigines, they are flat, clearly delineated, rounded and either brown, black or gray.
- If the dark pigmentation on your back is a reaction to inflammation or injury, there may be redness, scabs, scars or other signs of the body's healing process.
Diagnosis
A visual inspection, consideration of other symptoms, your medical history, your immediate family's medical history and an account of your sun exposure, sunburns and sun protection habits are key to diagnosing sun-related spots. Your dermatologist may take a sample of affected skin for biopsy, as well. Post-inflammatory hyperpigmentation is generally diagnosed with an examination and consideration of whether there was any recent injury, acne breakout or other problem in the area. A doctor performs an ACTH stimulation test to diagnose Addison's disease. This test measure the levels of the hormone cortisol in the blood and/or urine, explains the National Endocrine and Metabolic Diseases Information Service. A CRH stimulation test is used if abnormal results are produced by the first test.
- A visual inspection, consideration of other symptoms, your medical history, your immediate family's medical history and an account of your sun exposure, sunburns and sun protection habits are key to diagnosing sun-related spots.
- Your dermatologist may take a sample of affected skin for biopsy, as well.
Prevention
What Causes Blackheads on My Back?
Learn More
Solar lentigines are best prevented from appearing and from worsening by protecting the skin on your back from UV radiation. Forgo artificial tanning, advises the AgingSkinNet website of the American Academy of Dermatology 3. Wear a shirt made from tightly-knit fabric outdoors. If you won't be wearing a shirt, have someone apply a sunblock to your back about half an hour beforehand. Use a waterproof product if you are likely to swim or sweat. Post-inflammatory hyperpigmentation is less likely to occur if you refrain from scratching, picking at or otherwise aggravating injured skin. Addison's disease is usually the result of an autoimmune disorder, and is not typically preventable. However, proper management of known autoimmune conditions may help.
- Solar lentigines are best prevented from appearing and from worsening by protecting the skin on your back from UV radiation.
- Post-inflammatory hyperpigmentation is less likely to occur if you refrain from scratching, picking at or otherwise aggravating injured skin.
Treatment
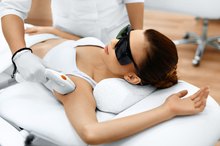
Any type of hyperpigmentation on the back may be faded with topical skin lightening agents. Hydroquinone products used in conjunction with retinoids and mild steroids is a leading course of treatment, according to MayoClinic.com 2. Cosmetic procedures, including cryotherapy, laser therapy, chemical peels and dermabrasion, can get rid of dark pigmentation as well. In addition, treatment of Addison's disease primarily consists of hormone replacement therapy.
- Any type of hyperpigmentation on the back may be faded with topical skin lightening agents.
- Cosmetic procedures, including cryotherapy, laser therapy, chemical peels and dermabrasion, can get rid of dark pigmentation as well.
Related Articles
References
- The Merck Manuals Online Medical Library: Hyperpigmentation
- MayoClinic.com: Age Spots (Liver Spots)
- AgingSkinNet: Age Spots
- American Academy of Dermatology. Variety of Options Available to Treat Pigmentation Problems. February 5, 2013. https://www.aad.org/media/news-releases/variety-of-options-available-to-treat-pigmentation-problems
- Tomecki J, Woodhouse G. Common Benign Growths. Cleveland Clinic Center for Continuing Education. http://www.clevelandclinicmeded.com/medicalpubs/diseasemanagement/dermatology/common-benign-growths/
- Scarcella G, Dethlefsen MW, Nielsen MCE. Treatment of solar lentigines using a combination of picosecond laser and biophotonic treatment. Clin Case Rep. 2018;6(9):1868-1870. doi:10.1002/ccr3.1749
- Scherer D, Kumar R. Genetics of pigmentation in skin cancer--a review. Mutat Res. 2010;705(2):141-53. doi:10.1016/j.mrrev.2010.06.002
- Bastiaens M, Hoefnagel J, Westendorp R, Vermeer BJ, Bouwes bavinck JN. Solar lentigines are strongly related to sun exposure in contrast to ephelides. Pigment Cell Res. 2004;17(3):225-9. doi:10.1111/j.1600-0749.2004.00131.x
- Davis EC, Callender VD. Postinflammatory hyperpigmentation: a review of the epidemiology, clinical features, and treatment options in skin of color. J Clin Aesthet Dermatol. 2010;3(7):20-31.
- George AO, Shittu OB, Enwerem E, Wachtel M, Kuti O. The incidence of lower mid-trunk hyperpigmentation (linea nigra) is affected by sex hormone levels. J Natl Med Assoc. 2005;97(5):685-8.
- Al-saif FM, Baqays AA, Alsaif HF, Alhumidi AA. Erythromelanosis follicularis faciei et colli with reticulated hyperpigmentation of the extremities. Clin Case Rep. 2017;5(10):1576-1579. doi:10.1002/ccr3.1095
- Dereure O. Drug-induced skin pigmentation. Epidemiology, diagnosis and treatment. Am J Clin Dermatol. 2001;2(4):253-62. doi:10.2165/00128071-200102040-00006
- Ammoury A, Michaud S, Paul C, et al. Photodistribution of blue-gray hyperpigmentation after amiodarone treatment: molecular characterization of amiodarone in the skin. Arch Dermatol. 2008;144(1):92-6. doi:10.1001/archdermatol.2007.25
- Jain A, Gupta N. Multifocal Bullous Fixed Drug Erruption Due To Phenytoin: A Lesson Learned! J Clin Diagn Res. 2015;9(12):OD04-5. doi:10.7860/JCDR/2015/15464.6908
- Mccarty M, Rosso JQ. Chronic administration of oral trimethoprim-sulfamethoxazole for acne vulgaris. J Clin Aesthet Dermatol. 2011;4(8):58-66.
- Massinde A, Ntubika S, Magoma M. Extensive hyperpigmentation during pregnancy: a case report. J Med Case Rep. 2011;5:464. doi:10.1186/1752-1947-5-464
- Sarkar SB, Sarkar S, Ghosh S, Bandyopadhyay S. Addison's disease. Contemp Clin Dent. 2012;3(4):484-6. doi:10.4103/0976-237X.107450
- Lause M, Kamboj A, Fernandez faith E. Dermatologic manifestations of endocrine disorders. Transl Pediatr. 2017;6(4):300-312. doi:10.21037/tp.2017.09.08
- Enguita FJ, Leitão AL. Hydroquinone: environmental pollution, toxicity, and microbial answers. Biomed Res Int. 2013;2013:542168. doi:10.1155/2013/542168
- Arora P, Sarkar R, Garg VK, Arya L. Lasers for treatment of melasma and post-inflammatory hyperpigmentation. J Cutan Aesthet Surg. 2012;5(2):93-103. doi:10.4103/0974-2077.99436
- Prohaska J, Badri T. Cryotherapy. StatPearls Publishing. 2019.
- Schalka S. New data on hyperpigmentation disorders. J Eur Acad Dermatol Venereol. 2017;31 Suppl 5:18-21. doi:10.1111/jdv.14411
- American Academy of Dermatology. Variety of Options Available to Treat Pigmentation Problems. February 5, 2013.
- Tomecki J, Woodhouse G. Common Benign Growths. Cleveland Clinic Center for Continuing Education.
Writer Bio
Eric Mohrman has been a freelance writer since 2007, focusing on travel, food and lifestyle stories. His creative writing is also widely published. He lives in Orlando, Florida.