Reddish-Brown Spots on the Skin
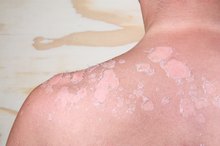
Reddish-brown spots on the skin can be due to a variety of conditions ranging from bruising and bleeding under the skin, to skin cancer and diseases such as psoriasis or eczema. According to the American Academy of Family Physicians, oftentimes reddish-brown spots are harmless changes that occur with age 4. They also can indicate more serious medical conditions that a dermatologist should inspect.
Considerations
Natural changes to the skin occur with age. Age spots, also called liver spots, appear as reddish-brown spots on areas exposed to the sun and usually are harmless. Also called lentigines or liver spots, they usually appear on the backs of the hands, the back, feet or face. Fade creams may reduce the appearance of age spots. When they develop unusual shapes, the spots should be evaluated for potential malignancies.
- Natural changes to the skin occur with age.
- Age spots, also called liver spots, appear as reddish-brown spots on areas exposed to the sun and usually are harmless.
Types
Dark Pigmentation on the Back
Learn More
A nerve infection that causes reddish-brown bumps on the body is called shingles and is common in the elderly, although it can affect people of any age. Early symptoms of shingles include fatigue, headaches or localized pain. The spots usually appear in a line across the chest, face, scalp, feet or hands. They usually stay on one side of the body. Shingles spots typically last for a couple weeks and are treated with anti-viral medications.
- A nerve infection that causes reddish-brown bumps on the body is called shingles and is common in the elderly, although it can affect people of any age.
Features
Bacterial and fungal infections are prevalent among people with diabetes and usually appear as reddish-brown spots around the eyelids, nails and hair follicles. The spots usually are itchy and also may appear in warm folds of the skin. According to the American Diabetes Organization, arc-shaped rashes that are reddish-brown and appear on the fingers or ears may be due to disseminated granuloma annulare and should be treated by a doctor 1.
Warning
Reasons for Purplish Skin on the Neck Area
Learn More
Small reddish-brown spots called actinic keratosis are first felt by touch rather than noticed by the eye and may prove to be precancerous skin cells. They can grow to about an eighth or quarter-inch in size and be sensitive or itchy. The spots can develop into a number of different skin cancers and may be removed by your doctor or treated with topical creams to make them dissolve.
Identification
Psoriasis is an autoimmune disease that produces reddish-brown scales and lesions on the skin. Sometimes the spots are covered with a buildup of white, silvery dead skin cells. Various conditions trigger psoriasis outbreaks and can include medications, an injury or stress. People with psoriasis also are at risk for developing skin cancers, diabetes and inflammatory bowel disease. According to the National Psoriasis Foundation, a healthy diet, stress-relieving practices and regular exercise are the most effective treatments to prevent outbreaks 3.
- Psoriasis is an autoimmune disease that produces reddish-brown scales and lesions on the skin.
Related Articles
References
- American Diabetes Organization: Skin Conditions
- Skin Cancer Foundation: Precancers
- National Psoriasis Foundation: About Psoriasis
- American Academy of Family Physicians: Mature Skin
- American Academy of Dermatology. Variety of Options Available to Treat Pigmentation Problems. February 5, 2013. https://www.aad.org/media/news-releases/variety-of-options-available-to-treat-pigmentation-problems
- Tomecki J, Woodhouse G. Common Benign Growths. Cleveland Clinic Center for Continuing Education. http://www.clevelandclinicmeded.com/medicalpubs/diseasemanagement/dermatology/common-benign-growths/
- Scarcella G, Dethlefsen MW, Nielsen MCE. Treatment of solar lentigines using a combination of picosecond laser and biophotonic treatment. Clin Case Rep. 2018;6(9):1868-1870. doi:10.1002/ccr3.1749
- Scherer D, Kumar R. Genetics of pigmentation in skin cancer--a review. Mutat Res. 2010;705(2):141-53. doi:10.1016/j.mrrev.2010.06.002
- Bastiaens M, Hoefnagel J, Westendorp R, Vermeer BJ, Bouwes bavinck JN. Solar lentigines are strongly related to sun exposure in contrast to ephelides. Pigment Cell Res. 2004;17(3):225-9. doi:10.1111/j.1600-0749.2004.00131.x
- Davis EC, Callender VD. Postinflammatory hyperpigmentation: a review of the epidemiology, clinical features, and treatment options in skin of color. J Clin Aesthet Dermatol. 2010;3(7):20-31.
- George AO, Shittu OB, Enwerem E, Wachtel M, Kuti O. The incidence of lower mid-trunk hyperpigmentation (linea nigra) is affected by sex hormone levels. J Natl Med Assoc. 2005;97(5):685-8.
- Al-saif FM, Baqays AA, Alsaif HF, Alhumidi AA. Erythromelanosis follicularis faciei et colli with reticulated hyperpigmentation of the extremities. Clin Case Rep. 2017;5(10):1576-1579. doi:10.1002/ccr3.1095
- Dereure O. Drug-induced skin pigmentation. Epidemiology, diagnosis and treatment. Am J Clin Dermatol. 2001;2(4):253-62. doi:10.2165/00128071-200102040-00006
- Ammoury A, Michaud S, Paul C, et al. Photodistribution of blue-gray hyperpigmentation after amiodarone treatment: molecular characterization of amiodarone in the skin. Arch Dermatol. 2008;144(1):92-6. doi:10.1001/archdermatol.2007.25
- Jain A, Gupta N. Multifocal Bullous Fixed Drug Erruption Due To Phenytoin: A Lesson Learned! J Clin Diagn Res. 2015;9(12):OD04-5. doi:10.7860/JCDR/2015/15464.6908
- Mccarty M, Rosso JQ. Chronic administration of oral trimethoprim-sulfamethoxazole for acne vulgaris. J Clin Aesthet Dermatol. 2011;4(8):58-66.
- Massinde A, Ntubika S, Magoma M. Extensive hyperpigmentation during pregnancy: a case report. J Med Case Rep. 2011;5:464. doi:10.1186/1752-1947-5-464
- Sarkar SB, Sarkar S, Ghosh S, Bandyopadhyay S. Addison's disease. Contemp Clin Dent. 2012;3(4):484-6. doi:10.4103/0976-237X.107450
- Lause M, Kamboj A, Fernandez faith E. Dermatologic manifestations of endocrine disorders. Transl Pediatr. 2017;6(4):300-312. doi:10.21037/tp.2017.09.08
- Enguita FJ, Leitão AL. Hydroquinone: environmental pollution, toxicity, and microbial answers. Biomed Res Int. 2013;2013:542168. doi:10.1155/2013/542168
- Arora P, Sarkar R, Garg VK, Arya L. Lasers for treatment of melasma and post-inflammatory hyperpigmentation. J Cutan Aesthet Surg. 2012;5(2):93-103. doi:10.4103/0974-2077.99436
- Prohaska J, Badri T. Cryotherapy. StatPearls Publishing. 2019.
- Schalka S. New data on hyperpigmentation disorders. J Eur Acad Dermatol Venereol. 2017;31 Suppl 5:18-21. doi:10.1111/jdv.14411
- American Academy of Dermatology. Variety of Options Available to Treat Pigmentation Problems. February 5, 2013.
- Tomecki J, Woodhouse G. Common Benign Growths. Cleveland Clinic Center for Continuing Education.
Writer Bio
Linda Ray is an award-winning journalist with more than 20 years reporting experience. She's covered business for newspapers and magazines, including the "Greenville News," "Success Magazine" and "American City Business Journals." Ray holds a journalism degree and teaches writing, career development and an FDIC course called "Money Smart."