What does fact checked mean?
At Healthfully, we strive to deliver objective content that is accurate and up-to-date. Our team periodically reviews articles in order to ensure content quality. The sources cited below consist of evidence from peer-reviewed journals, prominent medical organizations, academic associations, and government data.
The information contained on this site is for informational purposes only, and should not be used as a substitute for the advice of a professional health care provider. Please check with the appropriate physician regarding health questions and concerns. Although we strive to deliver accurate and up-to-date information, no guarantee to that effect is made.
Can You Get a Ringworm on the Mouth?
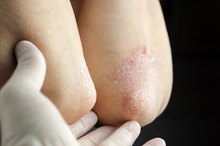
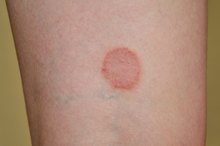
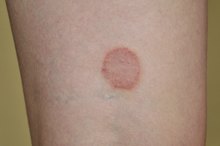
Contrary to its name, ringworm is not caused by worms but by a contagious fungal infection of the skin. It develops as a small, red, raised, round patch that gradually enlarges. The outer ring looks inflamed, while the inside appears to be healthy skin 2. The condition can develop anywhere on the skin’s dead top layer. Ringworm cannot occur in the mouth or any other area lined with mucous membranes.
If you are experiencing serious medical symptoms, seek emergency treatment immediately.
Cause
Ringworm is most often acquired by direct contact with an infected person or household pet. It can also be caught from touching a contaminated floor, shower or bathtub, or an infected object, such as a brush. Rarely, ringworm can be picked up from infected soil. Dermatophytes--microorganisms found pretty much everywhere--are the mold-like fungi that lead to ringworm.
- Ringworm is most often acquired by direct contact with an infected person or household pet.
- It can also be caught from touching a contaminated floor, shower or bathtub, or an infected object, such as a brush.
Diagnosis
How to Get Rid of Ringworm in 2 Days
Learn More
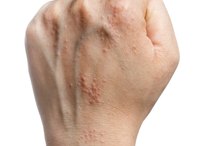
Ringworm’s distinct scaly, red and itchy ring-like rash generally makes self-diagnosis easy. Since the condition can spread, it’s common to notice more than one patch of ringworm on the body or red rings that overlap. A rash that doesn’t improve or disappear within two weeks--or that becomes excessively red, sore or pussy--may require a doctor visit and professional evaluation.
- Ringworm’s distinct scaly, red and itchy ring-like rash generally makes self-diagnosis easy.
- A rash that doesn’t improve or disappear within two weeks--or that becomes excessively red, sore or pussy--may require a doctor visit and professional evaluation.
Treatment
A nonprescription, topical, antifungal skin cream or ointment is the most common treatment. More severe cases may require a prescription cream or, in some cases, an antifungal drug that usually comes in tablet form. Covering the rash with clothing or an adhesive bandage can help prevent its spread.
Prevention
How to Get Rid of Ringworm in Seven Days
Learn More
Skin fungi grow best in moist, warm areas. To help prevent ringworm, keep your body dry. Wear loose-fitting underwear that won’t trap moisture, and change socks daily. Wear sandals or other protective footwear in moist areas, such as locker rooms, gyms and pools. Also, avoid sharing towels, combs and other personal items.
- Skin fungi grow best in moist, warm areas.
- Wear loose-fitting underwear that won’t trap moisture, and change socks daily.
Added insight
Other common skin conditions, including eczema and psoriasis, sometimes resemble ringworm, especially in its early stages when the ring is small. If you have questions or concerns--or if you experience a rash accompanied by fever--contact your doctor.
Related Articles
References
- Harvard Medical School Family Health Guide, 1999, President & Fellows of Harvard College
- National Institutes of Health: Tinea Infections
- Cornell University College of Veterinary Medicine. Ringworm: A Serious but Readily Treatable Affliction. 2018.
- Centers for Disease Control and Prevention. Ringworm Information for Healthcare Professionals. Updated February 6, 2020.
- Ely JW, Rosenfeld S, Seabury Stone M. Diagnosis and management of tinea infections. Am Fam Physician. 2014;90(10):702-710.
- American Academy of Dermatology. “Ringworm: Diagnosis, Treatment, and Outcome.”
- Laniosz V, Wetter DA. "What's New in the Treatment and Diagnosis of Dermatophytosis?" Seminars in Cutaneous Medicine and Surgery. 2014 Sep;33(3):136-9.
Writer Bio
Cynthia Wolfe Boynton is an award-winning writer and editor who has been freelancing since 1994. Her writing credits include "The New York Times," "Boston Globe," "Better Health" magazine, "Connecticut" magazine and drkoop.com, among other publications and Internet sites. A college English and journalism instructor, she runs several popular creative writing programs and has an extensive public relations background.