What does fact checked mean?
At Healthfully, we strive to deliver objective content that is accurate and up-to-date. Our team periodically reviews articles in order to ensure content quality. The sources cited below consist of evidence from peer-reviewed journals, prominent medical organizations, academic associations, and government data.
The information contained on this site is for informational purposes only, and should not be used as a substitute for the advice of a professional health care provider. Please check with the appropriate physician regarding health questions and concerns. Although we strive to deliver accurate and up-to-date information, no guarantee to that effect is made.
Ringworm in Babies
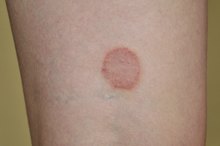
Ringworm is a contagious skin infection common among babies and children. The belief that ringworm is caused by worms is a widespread misconception. Ringworm is the common name for tinea corporis, a fungal infection, which forms ringlike patterns on the skin. The name ringworm comes from these rings, which can look like round worms below the skin's surface.
If you are experiencing serious medical symptoms, seek emergency treatment immediately.
Background
Ringworm infection is caused by a type of fungi called dermatophytes. Tinea is the medical name for dermatophyte infections. There are several types of tinea infections including tinea corporis, or ringworm of the body; tinea pedis, or athlete’s foot; tinea cruris, or jock itch, and tinea capitis, ringworm of the scalp. Tinea corporis and tinea capitis are most commonly seen in babies and children, although children can become infected with all four types of tinea.
- Ringworm infection is caused by a type of fungi called dermatophytes.
- Tinea corporis and tinea capitis are most commonly seen in babies and children, although children can become infected with all four types of tinea.
Causes
How Long Does It Take for Ringworm to Clear Up?
Learn More
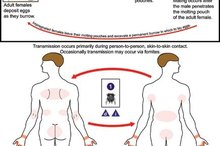
Your baby can become infected with ringworm through direct skin-to-skin contact with another infected person or through contact with the hands of an infected person who has been scratching the rash. Additionally, the fungus that causes ringworm can spread via contaminated personal items such as towels, clothing and bedding. Household pets, especially puppies and kittens, can also transfer ringworm to humans.
Symptoms
Babies with ringworm will present with slightly red, round, raised lesions over the face, trunk, or limbs. These lesions typically have a border consisting of small scales, blisters or bumps. The skin between lesions and in the center of lesions usually appears normal. Lesions can vary in size from about the size of a dime to several inches across. Lesions that are close to each other may come together, taking on a multilobed appearance. One of the most common symptoms of ringworm is itching at the infection site. Other symptoms can include redness, burning, scaling or fissuring of the skin. If the scalp is infected, hair loss may also occur.
- Babies with ringworm will present with slightly red, round, raised lesions over the face, trunk, or limbs.
- Other symptoms can include redness, burning, scaling or fissuring of the skin.
Treatment
Itchiness Behind the Ears
Learn More
According to AskDrSears.com, the standard treatment for ringworm is an over-the-counter antifungal cream called clotrimazole, commonly known as Lotrimin or Mycelex 2. Clotrimazole should be applied to the affected areas and surrounding skin twice daily. Typically, babies will require at least two weeks of treatment. While most cases of ringworm are treated with over-the-counter medications, your pediatrician will tell you which treatment is right for your child. If the rash has not improved after two weeks of treatment, your pediatrician may decide to treat with a three- to four-week course of oral anti-fungal medication, such as griseofulvin and terbinafine.
- According to AskDrSears.com, the standard treatment for ringworm is an over-the-counter antifungal cream called clotrimazole, commonly known as Lotrimin or Mycelex 2.
- If the rash has not improved after two weeks of treatment, your pediatrician may decide to treat with a three- to four-week course of oral anti-fungal medication, such as griseofulvin and terbinafine.
Prevention
One of the easiest ways to prevent the spread of ringworm is proper handwashing. Parents and caregivers should wash their hands after contact with infected children. Infected children should also have their hands cleaned regularly and should be encouraged not to scratch at lesions. If necessary, infant mittens can be used with babies to keep them from scratching. All blankets, clothing, towels, hats and other personal items used by your baby prior to treatment need to be washed in hot water or discarded. Babies with ringworm are no longer considered contagious after 48 hours of treatment.
- One of the easiest ways to prevent the spread of ringworm is proper handwashing.
- If necessary, infant mittens can be used with babies to keep them from scratching.
Related Articles
References
- Skinsight: Ringworm (Tinea Corporis) A Parent's Guide to Condition and Treatment Information
- AskDr.Sears.com: Ringworm
- Homei A, Worboys M. Fungal Disease in Britain and the United States 1850–2000: Mycoses and Modernity. Basingstoke (UK): Palgrave Macmillan; 2013. Chapter 1, Ringworm: A Disease of Schools and Mass Schooling. Available from: https://www.ncbi.nlm.nih.gov/books/NBK169210/
- Jain A, Jain S, Rawat S. Emerging fungal infections among children: A review on its clinical manifestations, diagnosis, and prevention. J Pharm Bioallied Sci. 2010;2(4):314–320. doi:10.4103/0975-7406.72131
- Yee G, Al Aboud AM. Tinea Corporis. [Updated 2019 Jul 6]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK544360/
- Alkeswani A, Duncan JR, Theos A. Tinea faciei starting at day two of life. Pediatr Dermatol. 2019;36(1):e20-e22.
- Furlan KC, Kakizaki P, Chartuni JC, Valente NY. Sycosiform tinea barbae caused by trichophyton rubrum and its association with autoinoculation. An Bras Dermatol. 2017;92(1):160–161. doi:10.1590/abd1806-4841.20174802
- Hay RJ. Tinea Capitis: Current Status. Mycopathologia. 2017;182(1-2):87–93. doi:10.1007/s11046-016-0058-8
- InformedHealth.org [Internet]. Cologne, Germany: Institute for Quality and Efficiency in Health Care (IQWiG); 2006-. Athlete's foot: Overview. 2015 Jan 14 [Updated 2018 Jun 14].Available from: https://www.ncbi.nlm.nih.gov/books/NBK279549/
- Nadalo D, Montoya C, Hunter-smith D. What is the best way to treat tinea cruris?. J Fam Pract. 2006;55(3):256-8.
- Das S, Barbhuniya JN, Biswas I, Bhattacharya S, Kundu PK. Studies on comparison of the efficacy of terbinafine 1% cream and butenafine 1% cream for the treatment of Tinea cruris. Indian Dermatol Online J. 2010;1(1):8–9. doi:10.4103/2229-5178.73249
- Errichetti E, Stinco G. Dermoscopy in tinea manuum. An Bras Dermatol. 2018;93(3):447–448. doi:10.1590/abd1806-4841.20186366
- Piraccini BM, Alessandrini A. Onychomycosis: A Review. J Fungi (Basel). 2015;1(1):30–43. Published 2015 Mar 27. doi:10.3390/jof1010030
- Ashraf M, Biswas J. Chronic ringworm infestation and Marjolin's ulcer, an association unknown in the literature. Rare Tumors. 2010;2(2):e31. Published 2010 Jun 30. doi:10.4081/rt.2010.e31
- Landry GL, Chang CJ, Mees PD. Treating and avoiding herpes and tinea infections in contact sports. Phys Sportsmed. 2004;32(10):43-4.
- Davis EC, Callender VD. Postinflammatory hyperpigmentation: a review of the epidemiology, clinical features, and treatment options in skin of color. J Clin Aesthet Dermatol. 2010;3(7):20–31.
- Fuller LC, Child FJ, Midgley G, Higgins EM. Diagnosis and management of scalp ringworm. BMJ. 2003;326(7388):539–541. doi:10.1136/bmj.326.7388.539
- Boral H, Durdu M, Ilkit M. Majocchi's granuloma: current perspectives. Infect Drug Resist. 2018;11:751–760. Published 2018 May 22. doi:10.2147/IDR.S145027
- Al Aboud AM, Crane JS. Tinea Capitis. [Updated 2019 Mar 2]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK536909/
- Ely JW, Rosenfeld S, Seabury stone M. Diagnosis and management of tinea infections. Am Fam Physician. 2014;90(10):702-10.
- “Ringworm: Signs and Symptoms.” American Academy of Dermatology, American Academy of Dermatology.
- Laniosz V, Wetter DA. "What's New in the Treatment and Diagnosis of Dermatophytosis?" Seminars in Cutaneous Medicine and Surgery. 2014 Sep;33(3):136-9.
Writer Bio
Kimberley Zagoren has been writing since 2002. With experience in pediatric and neonatal intensive care nursing, Zagoren writes for several online sources, such as eHow, focusing primarily on health-related issues. She received her Associate of Science in nursing degree from Middlesex College.