What does fact checked mean?
At Healthfully, we strive to deliver objective content that is accurate and up-to-date. Our team periodically reviews articles in order to ensure content quality. The sources cited below consist of evidence from peer-reviewed journals, prominent medical organizations, academic associations, and government data.
The information contained on this site is for informational purposes only, and should not be used as a substitute for the advice of a professional health care provider. Please check with the appropriate physician regarding health questions and concerns. Although we strive to deliver accurate and up-to-date information, no guarantee to that effect is made.
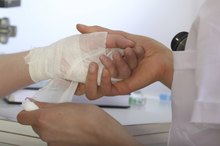
How to Treat a Burn on the Fingers
A burn is always uncomfortable and often painful. This is especially true when the burn is on your hands or fingers, which are used frequently. For minor burns, taking these steps can soothe the pain and promote healing.
Immediately run your burned finger(s) under cool (not cold) water. This will stop the actual burning sensation and will soothe the affected area. Fill a bowl with cool water and rest your hand in it for ongoing relief.
How to Treat Muffler Burns
Learn More
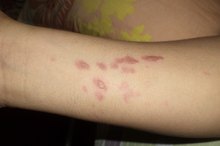
Look for any skin damage. A mild burn is characterized by red skin and sometimes small blisters 1. You can treat a mild burn at home. However, if you have a severe burn (large blistering, charred skin, peeling skin), seek medical attention immediately.
Apply an over-the-counter, topical burn ointment to your burn. Cover your hands/fingers with a non-sticky bandage. This will minimize the chance for infection. Change your bandages at least once a day.
How to Treat a Salicylic Acid Burn
Learn More
Take an over-the-counter pain reliever, such as ibuprofen or acetaminophen, to reduce discomfort.
Drink plenty of water. One of the side effects of burns is dehydration, so make sure to keep yourself hydrated.
Tips
If your hands or fingers become very swollen, numb, tingly, cold or even blue, seek medical attention. Severe swelling may cause blood-flow restriction, which is dangerous.
Warnings
Avoid wearing gloves or shirts that restrict blood flow or irritate the skin. Do not apply butter or an oil-based lotion or ointment to the burn; this will cause further irritation.
Related Articles
References
- MedlinePlus: Medical Encyclopedia
- Cuttle L, Pearn J, McMillan JR, Kimble RM. A review of first aid treatments for burn injuries. Burns. 2009;35(6):768-775. doi:10.1016/j.burns.2008.10.011
- Lloyd ECO, Rodgers BC, Michener M, Williams MS. Outpatient burns: prevention and care. Am Fam Physician. 2012;85(1):25-32.
- Shrivastava P, Goel A. Pre-hospital care in burn injury. Indian J Plast Surg. 2010;43(Suppl):S15-S22. doi:10.4103/0970-0358.70720
- Nielson CB, Duethman NC, Howard JM, Moncure M, Wood JG. Burns: Pathophysiology of Systemic Complications and Current Management. J Burn Care Res. 2017;38(1):e469-e481. doi:10.1097/BCR.0000000000000355
- Schaefer TJ, Tannan SC. Thermal Burns. In: StatPearls. Treasure Island, FL: StatPearls Publishing; 2019.
- Cancio LC, Barillo DJ, Kearns RD, et al. Guidelines for Burn Care Under Austere Conditions: Surgical and Nonsurgical Wound Management. J Burn Care Res. 2017;38(4):203-214. doi:10.1097/BCR.0000000000000368
- Lloyd ECO, Rodgers BC, Michener M, Williams MS. Outpatient burns: prevention and care. Am Fam Physician. 2012;85(1):25-32.
- Munteanu A, Florescu IP, Nitescu C. A modern method of treatment: The role of silver dressings in promoting healing and preventing pathological scarring in patients with burn wounds. J Med Life. 2016;9(3):306-315.
Tips
- If your hands or fingers become very swollen, numb, tingly, cold or even blue, seek medical attention. Severe swelling may cause blood-flow restriction, which is dangerous.
Warnings
- Avoid wearing gloves or shirts that restrict blood flow or irritate the skin.
- Do not apply butter or an oil-based lotion or ointment to the burn; this will cause further irritation.
Writer Bio
Wendy Rose Gould is a professional journalist who has contributed to "Glamour" magazine and the Huffington Post, among other publications. After internships at the "Indianapolis Business Journal," "Kiwanis International" and "NUVO Newsweekly," she earned BA degrees in journalism and philosophy from Franklin College in 2008. Gould specializes in lifestyle topics.