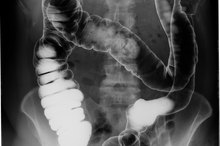
Air Pocket After a Colonoscopy
The main purpose of the colonoscopy screening test is to help doctors detect and potentially treat problems in the colon before they become something serious (such as cancer). A colonoscopy can also help doctors determine what's causing digestive symptoms such as unexplained weight loss, rectal bleeding, abdominal pain or sudden changes in bowel habits. (According to the American Cancer Society, these can all be signs of cancer, but are more commonly caused by something less serious, such as an infection, hemorrhoids, irritable bowel syndrome or inflammatory bowel disease. 5)
A colonoscopy typically takes 20 to 60 minutes to complete, and involves having a doctor insert a colonoscope — a long, thin flexible tube that has a camera at one end — through the anus to examine the entire colon. The doctor will give you sedation beforehand, so you shouldn't feel anything while it's happening, say doctors at the Dana-Farber Cancer Institute 1. Afterwards, however, you may experience some discomfort.
Two of the most common side effects of a colonoscopy are bloating and cramping from gas that has collected in the abdomen during the procedure. This is completely normal, according to experts at Johns Hopkins Medicine 8. The gassiness is usually harmless, but it can be quite uncomfortable. Fortunately, there are some easy ways to feel better fast.
What Causes Gassiness After a Colonoscopy?
During a colonoscopy, the doctor will pump either carbon dioxide or air into the colon in order to inflate it and make it easier to see the colon with the colonoscope. This air forms air pockets that can create some of the annoying post-colonoscopy symptoms. “It will cause them gas pains.”
Today, more and more doctors are using carbon dioxide instead of air to expand the colon. Studies have shown that using carbon dioxide usually results in less gas retention, and therefore “greatly decreases the chances of having [gas] pain [afterward],” says Dr. Ashcraft.
- During a colonoscopy, the doctor will pump either carbon dioxide or air into the colon in order to inflate it and make it easier to see the colon with the colonoscope.
How to Treat Post-Colonoscopy Gassiness
Abdominal Pain After Colonoscopy
Learn More
You can also treat post-colonoscopy gassiness by taking a medication called simethicone, available in over-the-counter products such as:
- Gas-X
- Phazyme Maximum Strength
- Mytab Gas Multiple Strength
- Maalox Anti-Gas
- Alka-Seltzer Anti-Gas
But even though these drugs may provide quick relief, “getting up and walking around is far more efficient” when it comes to alleviating colonoscopy-induced gas pains, says Dr. Ashcraft. (By the time a gas-relief pill has traveled all the way to your colon, you could already have released a large amount of gas just by walking, he points out.)
Related Articles
References
- Dana-Farber Cancer Institute: “Understanding upper endoscopy and colonoscopy.”
- Mayo Clinic: "Simethicone (Oral Route)."
- National Library of Medicine: "Simethicone."
- John Ashcraft, DO, associate professor of surgery and chief of colon and rectal surgery, University of Kansas Medical Center, Kansas City
- American Cancer Society: "Signs and Symptoms of Colorectal Cancer."
- Massachusetts General Hospital: "Colonoscopy Bowel Preparation Instructions ."
- University of Michigan: "Simethicone."
- Johns Hopkins Medicine: "Colonoscopy."
- Niikura R, Hirata Y, Suzuki N, et al. Colonoscopy reduces colorectal cancer mortality: A multicenter, long-term, colonoscopy-based cohort study. PLoS One. 2017;12(9):e0185294. doi:10.1371/journal.pone.0185294
- American Society for Gastrointestinal Endoscopy. Understanding Polyps and Their Treatment.
- National Institute of Diabetes and Digestive and Kidney Diseases. Colonoscopy. Updated July 2017.
- American Cancer Society. Signs and Symptoms of Colorectal Cancer. Updated February 25, 2019.
- Johns Hopkins Medicine. Colonoscopy.
- Jayasekeran V, Holt B, Bourke M. Normal Adult Colonic Anatomy in Colonoscopy. Video Journal and Encyclopedia of GI Endoscopy. 2013;1(2):390-392. doi:10.1016/s2212-0971(13)70173-0.
- Johns Hopkins Medicine. Virtual Colonoscopy.
- Pickhardt PJ, Pooler BD, Mbah I, Weiss JM, Kim DH. Colorectal Findings at Repeat CT Colonography Screening after Initial CT Colonography Screening Negative for Polyps Larger than 5 mm. Radiology. 2017;282(1):139-148. doi:10.1148/radiol.2016160582.
- National Cancer Institute. Tests to Detect Colorectal Cancer and Polyps. Updated July 7, 2016.
- Shariff MK, Sheikh K, Carroll NR, et al. Colorectal cancer detection: time to abandon barium enema? Frontline Gastroenterol. 2011;2(2):105–109. doi:10.1136/fg.2010.003616
- Zapka J, Klabunde CN, Taplin S, Yuan G, Ransohoff D, Kobrin S. Screening colonoscopy in the US: attitudes and practices of primary care physicians. J Gen Intern Med. 2012;27(9):1150–1158. doi:10.1007/s11606-012-2051-3
- Moon W. Optimal and safe bowel preparation for colonoscopy. Clin Endosc. 2013;46(3):219–223. doi:10.5946/ce.2013.46.3.219
- Kim SY, Kim HS, Park HJ. Adverse events related to colonoscopy: Global trends and future challenges. World J Gastroenterol. 2019;25(2):190–204. doi:10.3748/wjg.v25.i2.190
- Hamdani U, Naeem R, Haider F, et al. Risk factors for colonoscopic perforation: a population-based study of 80118 cases. World J Gastroenterol. 2013;19(23):3596-601. doi:10.3748/wjg.v19.i23.3596
- Jehangir A, Bennett KM, Rettew AC, Fadahunsi O, Shaikh B, Donato A. Post-polypectomy electrocoagulation syndrome: a rare cause of acute abdominal pain. J Community Hosp Intern Med Perspect. 2015;5(5):29147. doi:10.3402/jchimp.v5.29147
- Bhagatwala J, Singhal A, Aldrugh S, Sherid M, Sifuentes H, Sridhar S. Colonoscopy — Indications and Contraindications. Screening for Colorectal Cancer with Colonoscopy. February 2015. doi:10.5772/61097.
- Ahmed M. Blood thinners and gastrointestinal endoscopy. World J Gastrointest Endosc. 2016;8(17):584–590. doi:10.4253/wjge.v8.i17.584
- University of Connecticut Health. Medications to Avoid for GI Endoscopy Procedures.
- Ghisi D, Fanelli A, Tosi M, Nuzzi M, Fanelli G. Monitored anesthesia care. Minerva Anestesiol. 2005;71(9):533-8.
- Rundshagen I. Postoperative cognitive dysfunction. Dtsch Arztebl Int. 2014;111(8):119–125. doi:10.3238/arztebl.2014.0119
- De'angelis N, Di saverio S, Chiara O, et al. 2017 WSES guidelines for the management of iatrogenic colonoscopy perforation. World J Emerg Surg. 2018;13:5. doi:10.1186/s13017-018-0162-9
Writer Bio
Esther Kinuthia is a registered nurse with extensive experience in health and wellness. She holds a B.S. in nursing, B.A in psychology and has worked for more than ten years in the health-care field. She enjoys writing articles on a variety of topics for the Internet. Her work has been published in various websites.