What does fact checked mean?
At Healthfully, we strive to deliver objective content that is accurate and up-to-date. Our team periodically reviews articles in order to ensure content quality. The sources cited below consist of evidence from peer-reviewed journals, prominent medical organizations, academic associations, and government data.
The information contained on this site is for informational purposes only, and should not be used as a substitute for the advice of a professional health care provider. Please check with the appropriate physician regarding health questions and concerns. Although we strive to deliver accurate and up-to-date information, no guarantee to that effect is made.
Salicylic Acid & Eczema
According to the American Academy of Allergy Asthma and Immunology, eczema affects between ten and 20 percent of children and between one and three percent of adults 1. Eczema, also known as atopic dermatitis, often begins in childhood and continues into adulthood 2. Many treatment options exist for eczema including self care, medications and allergy minimization. While usually not serious, eczema is bothersome and open skin wounds can become infected. Salicylic acid can be used to treat dry, flaky skin disorders such as eczema 3.
What is Salicylic Acid
Common scaly skin disorders can be treated with a medicine called salicylic acid, which is a topical preparation and may be used in conjunction with other medicines and treatments 3. Depending on the condition you are treating, you can get salicylic acid in doses ranging from 0.5% to 30% 3.
Treating Eczema
Light Brown Flaky Discoloration on the Skin
Learn More
When treating eczema, you can use a solution of salicylic acid to soften keratin, which is a protein that is part of the skin structure 3. Salicylic acid will help loosen the dry skin and take off the top layer of skin 3. This allows other topical medicines to penetrate better.
Salicylic Acid Side Effects
Mild side effects of salicylic acid can include skin irritation especially if the skin is broken or sensitive in the area you have applied it 3. More serious side effects include severe skin irritation, flushing and unusual warmth and redness of the skin. While not common, salicylic acid poisoning is possible and symptoms include:
- confusion
- diarrhea
- nausea
- dizziness
- headache
- rapid breathing
- ringing in ears
- severe drowsiness 3
Eczema Symptoms
What Is the Difference Between Stasis Dermatitis & Cellulitis?
Learn More
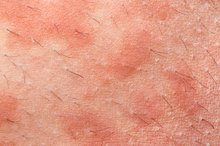
Eczema often appears on your arms and behind your knees. It can also show up anywhere else on your body including your face and neck. Usually it will show up as a red, itchy rash with cracked or scaly skin. You may have small, raised bumps that leak fluid and crust over. Eczema rashes are often itchy, especially at night. Most often, infants and children get eczema but it can continue into adulthood.
Most of the time, eczema comes and goes.
- Eczema often appears on your arms and behind your knees.
Eczema Treatments
Allergy control does not always eliminate eczema but it can reduce the extent of flare-ups. You can try to avoid or regularly clean items that trap dust such as:
- carpets
- stuffed toys
- pillows
- mattresses
- down comforters
- drapes
MayoClinic.com suggests using unscented soaps, moisturizers and calamine lotion, cool showers, and humidifiers to reduce eczema 2.
Related Articles
References
- American Academy of Allergy Asthma and Immunology: Allergy Statistics
- MayoClinic.com: Atopic Dermatitis (eczema)
- DermNet NZ: Salicylic acid
- Dermatology Online Journal: Treatment of molluscum contagiousum: A brief review and discussion of a case successfully treated with adapelene
- Arif T. "Salicylic acid as a peeling agent: a comprehensive review." Clinical Cosmetic and Investigational Dermatology. 2015 Aug; 8:455-61.
- Arif T. "Salicylic Acid as a Peeling Agent: A Comprehensive Review." Clinical Cosmetic and Investigational Dermatology. 2015 Aug 26;8:455-61.
- Castillo DE, Keri JE. "Chemical Peels in the Treatment of Acne: Patient Selection and Perspectives." Clinical Cosmetic and Investigational Dermatology. 2018; 11: 365–372.
- Zaenglein AL, Pathy AL, Schlosser BJ, et al. "Guidelines of Care for the Management of Acne Vulgaris."Journal of the American Academy of Dermatology. 2016 May;74(5):945-73.
Writer Bio
Tamara Laschinsky began writing articles in 2008 to supplement her knowledge of alternative health and wellness practices. Her articles have been re-published on various websites and requested by readers across the globe. She holds a degree in business administration from Red River College.