Signs & Symptoms Hypoglycemia & Hyperglycemia
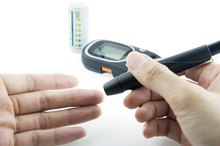
More than 23 million children and adults in the United States have diabetes, and each year 1.6 million people receive a new diagnosis of this disease, according to the American Diabetes Association. People with diabetes must carefully manage their blood sugar, or blood glucose, levels with diet, physical activity and medication to prevent diabetes complications and avoid hypoglycemia and hyperglycemia.
Hypoglycemia
When blood sugar levels drop below normal levels, a person may experience symptoms of hypoglycemia, such as nervousness, shakiness and hunger. He may sweat and feel dizzy, lightheaded and confused. Sleepiness, anxiety, confusion and difficulty talking are also signs that a person has hypoglycemia. A person who has hypoglycemia while sleeping may sweat profusely during sleep, experience nightmares or wake feeling tired and irritable. If hypoglycemia isn’t treated, the condition can worsen, causing more-severe symptoms such as fainting, confusion, clumsiness, seizures, coma and even death. According to the National Diabetes Information Clearinghouse, most cases of hypoglycemia are mild, and consuming food or drink rich in carbohydrates helps bring blood sugar levels back to normal. People with diabetes may need to take glucose tablets to raise their blood sugar levels quickly and avoid hypoglycemia's complications.
- When blood sugar levels drop below normal levels, a person may experience symptoms of hypoglycemia, such as nervousness, shakiness and hunger.
Hyperglycemia
How to Rid the Body of Carbon Dioxide
Learn More
Hyperglycemia, or high blood sugar levels, occur when the body lacks insulin or cannot use insulin properly. High levels of sugar in the urine indicate hyperglycemia; frequently feeling thirsty and having to urinate often are also indicators of high blood sugar levels. According to the American Diabetes Association, checking blood sugar levels often can help alert you to hyperglycemia before you feel symptoms. In many cases, reducing food intake and exercising can lower blood sugar levels, though you should not exercise if you have blood sugar levels above 240 mg/dL.
- Hyperglycemia, or high blood sugar levels, occur when the body lacks insulin or cannot use insulin properly.
- High levels of sugar in the urine indicate hyperglycemia; frequently feeling thirsty and having to urinate often are also indicators of high blood sugar levels.
Ketoacidosis
If hyperglycemia remains untreated, a person may develop ketoacidosis. In ketoacidosis, the lack of insulin in the body leads to the production of ketones, acids created when your body must burn fat instead of glucose that are excreted in your urine. You may develop a dry mouth, fruity-smelling breath and experience nausea and vomiting. If ketoacidosis isn’t treated, the person may develop constant fatigue, dry or flushed skin and confusion. High levels of ketones in your body can cause diabetic coma and, without treatment, even death. People with ketoacidosis usually need hospital treatment.
- If hyperglycemia remains untreated, a person may develop ketoacidosis.
- If ketoacidosis isn’t treated, the person may develop constant fatigue, dry or flushed skin and confusion.
Related Articles
References
- Mayo Clinic. Hyperglycemia in Diabetes. Apr 18, 2015.
- National Institute of Diabetes and Digestive and Kidney Diseases. The A1CTest & Diabetes. Apr 2018.
- Managing your blood sugar: MedlinePlus Medical Encyclopedia. MedlinePlus. May 17, 2018.
- Mouri M, Badireddy M. Hyperglycemia. Treasure Island, Fl: StatPearls Publishing; 2019.
- Okano J, Kojima H, Katagi M, et al. Hyperglycemia Induces Skin Barrier Dysfunctions with Impairment of Epidermal Integrity in Non-Wounded Skin of Type 1 Diabetic Mice. PLoS ONE. 2016;11(11):e0166215. doi:10.1371/journal.pone.0166215
- Maiorino MI, Bellastella G, Esposito K. Diabetes and sexual dysfunction: current perspectives. Diabetes Metab Syndr Obes. 2014;7:95-105. doi:10.2147/DMSO.S36455
- Mirghani dirar A, Doupis J. Gestational diabetes from A to Z. World J Diabetes. 2017;8(12):489-511. doi:10.4239/wjd.v8.i12.489
- Family Health History and Diabetes | CDC. Centers for Disease Control and Prevention. Jul 18, 2017.
- Farrar D. Hyperglycemia in pregnancy: prevalence, impact, and management challenges. Int J Womens Health. 2016;8:519-527. doi:10.2147/IJWH.S102117
- Goyal N, Kaur R, Sud A, Ghorpade N, Gupta M. Non Diabetic and Stress Induced Hyperglycemia [SIH] in Orthopaedic Practice What do we know so Far?. J Clin Diagn Res. 2014;8(10):LH01-3. doi:10.7860/JCDR/2014/10027.5022
- Riddell M, Perkins BA. Exercise and glucose metabolism in persons with diabetes mellitus: perspectives on the role for continuous glucose monitoring. J Diabetes Sci Technol. 2009;3(4):914-23. doi:10.1177/193229680900300439
- Sari MI, Sari N, Darlan DM, Prasetya RJ. Cigarette Smoking and Hyperglycaemia in Diabetic Patients. Open Access Maced J Med Sci. 2018;6(4):634-637. doi:10.3889/oamjms.2018.140
- Medagama AB. The glycaemic outcomes of Cinnamon, a review of the experimental evidence and clinical trials. Nutr J. 2015;14:108. doi:10.1186/s12937-015-0098-9
- Pramlintide Injection: MedlinePlus Drug Information. MedlinePlus. July 15, 2018.
- U.S. Food and Drug Administration. FDA Alerts Patients and Health Care Professionals to Nitrosamine Impurity Finding in Certain Metformin Extended-Release Products. May 28, 2020
- American Diabetes Association. High Blood Glucose. Mar 21, 2017.
- Mayo Clinic. Hyperglycemia in Diabetes. Apr 18, 2015.
- MedlinePlus. Metformin. Mar 15, 2020.
- National Institute of Diabetes and Digestive and Kidney Diseases. The A1CTest & Diabetes. Apr 2018.
Resources
Writer Bio
Amelia Smith is a freelance writer and editor who specializes in writing about fitness, nutrition, parenting, health, and medicine. She has a decade's worth of experience editing for online and print publications, including Parenting, Glamour, and Woman's Day. She obtained her Bachelor of Arts from the University of Hawaii.