What if an Age Spot Is Changing & Itchy?
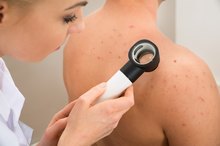
Everyday exposure to the sun takes its toll on your skin over the years, commonly manifesting in the form of age spots. These flat spots develop when color-producing cells in your skin multiply due to long-term exposure to ultraviolet radiation from the sun.
They often resemble large freckles and usually appear in areas that receive the most sun exposure, such as your face, forearms, shoulders and backs of your hands. Age spots are not cancerous, and they do not normally cause itchiness or other symptoms. But age spots can resemble cancerous or precancerous skin growths.
Warnings
See your doctor if you have an age spot that is itchy and/or changing in appearance to be sure it is not skin cancer or another type of growth that could turn into skin cancer.
Read more: 10 Foods That Are Linked to a Higher Cancer Risk
Age Spot Versus Skin Cancer
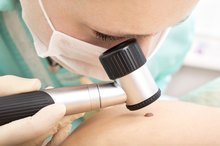
Though it can be difficult to tell an age spot apart from skin cancer, there are several subtle ways you can differentiate between the two. When in doubt, though, always consult your doctor. Here are three signs to check for:
Rate of Growth
Age spots typically develop slowly and can gradually increase in size over time. If you have several age spots in one area, some may eventually blend together to form larger spots. Cancerous and precancerous skin spots also grow over time, usually at a faster rate than age spots and with other changes in appearance.
Color 3
Age spots can range in color from yellowish to dark brown. The shades are often variable within the same spot, which is also a characteristic of the most dangerous type of skin cancer, melanoma. However, melanoma often has a greater range of color that may include shades of red, white and/or blue in addition to tan or brown.
Itchiness and Other Symptoms
While age spots do not cause itchiness, it's possible to have an itchy age spot for other reasons. For example, your skin may be sensitive to a new soap, making the age spots itchy.
While there may be another explanation for age spot itchiness, it could also be that what appears to be an age spot is actually something more serious. Skin cancer and precancerous skin spots often cause itchiness and may bleed easily, so it's important not to ignore these symptoms.
Read more: Can a Vitamin B-12 Deficiency Cause Itchy Skin?
Tips
Age spots are harmless and do not require treatment, but they can be an annoyance. Talk with your doctor if you are interested in cosmetic therapies to diminish the appearance of age spots.
- Though it can be difficult to tell an age spot apart from skin cancer, there are several subtle ways you can differentiate between the two.
- Skin cancer and precancerous skin spots often cause itchiness and may bleed easily, so it's important not to ignore these symptoms.
Related Articles
References
- Pathology of Melanocytic Nevi and Melanoma; Raymond Barnhill, et al.
- Sun Protection in Man; Paolo Giacomoni
- Color Atlas of Melanocytic Lesions of the Skin; H. Peter Soyer, et al.
- American Family Physician: Common Pigmentation Disorders
- American Academy of Dermatology. Variety of Options Available to Treat Pigmentation Problems. February 5, 2013. https://www.aad.org/media/news-releases/variety-of-options-available-to-treat-pigmentation-problems
- Tomecki J, Woodhouse G. Common Benign Growths. Cleveland Clinic Center for Continuing Education. http://www.clevelandclinicmeded.com/medicalpubs/diseasemanagement/dermatology/common-benign-growths/
- Scarcella G, Dethlefsen MW, Nielsen MCE. Treatment of solar lentigines using a combination of picosecond laser and biophotonic treatment. Clin Case Rep. 2018;6(9):1868-1870. doi:10.1002/ccr3.1749
- Scherer D, Kumar R. Genetics of pigmentation in skin cancer--a review. Mutat Res. 2010;705(2):141-53. doi:10.1016/j.mrrev.2010.06.002
- Bastiaens M, Hoefnagel J, Westendorp R, Vermeer BJ, Bouwes bavinck JN. Solar lentigines are strongly related to sun exposure in contrast to ephelides. Pigment Cell Res. 2004;17(3):225-9. doi:10.1111/j.1600-0749.2004.00131.x
- Davis EC, Callender VD. Postinflammatory hyperpigmentation: a review of the epidemiology, clinical features, and treatment options in skin of color. J Clin Aesthet Dermatol. 2010;3(7):20-31.
- George AO, Shittu OB, Enwerem E, Wachtel M, Kuti O. The incidence of lower mid-trunk hyperpigmentation (linea nigra) is affected by sex hormone levels. J Natl Med Assoc. 2005;97(5):685-8.
- Al-saif FM, Baqays AA, Alsaif HF, Alhumidi AA. Erythromelanosis follicularis faciei et colli with reticulated hyperpigmentation of the extremities. Clin Case Rep. 2017;5(10):1576-1579. doi:10.1002/ccr3.1095
- Dereure O. Drug-induced skin pigmentation. Epidemiology, diagnosis and treatment. Am J Clin Dermatol. 2001;2(4):253-62. doi:10.2165/00128071-200102040-00006
- Ammoury A, Michaud S, Paul C, et al. Photodistribution of blue-gray hyperpigmentation after amiodarone treatment: molecular characterization of amiodarone in the skin. Arch Dermatol. 2008;144(1):92-6. doi:10.1001/archdermatol.2007.25
- Jain A, Gupta N. Multifocal Bullous Fixed Drug Erruption Due To Phenytoin: A Lesson Learned! J Clin Diagn Res. 2015;9(12):OD04-5. doi:10.7860/JCDR/2015/15464.6908
- Mccarty M, Rosso JQ. Chronic administration of oral trimethoprim-sulfamethoxazole for acne vulgaris. J Clin Aesthet Dermatol. 2011;4(8):58-66.
- Massinde A, Ntubika S, Magoma M. Extensive hyperpigmentation during pregnancy: a case report. J Med Case Rep. 2011;5:464. doi:10.1186/1752-1947-5-464
- Sarkar SB, Sarkar S, Ghosh S, Bandyopadhyay S. Addison's disease. Contemp Clin Dent. 2012;3(4):484-6. doi:10.4103/0976-237X.107450
- Lause M, Kamboj A, Fernandez faith E. Dermatologic manifestations of endocrine disorders. Transl Pediatr. 2017;6(4):300-312. doi:10.21037/tp.2017.09.08
- Enguita FJ, Leitão AL. Hydroquinone: environmental pollution, toxicity, and microbial answers. Biomed Res Int. 2013;2013:542168. doi:10.1155/2013/542168
- Arora P, Sarkar R, Garg VK, Arya L. Lasers for treatment of melasma and post-inflammatory hyperpigmentation. J Cutan Aesthet Surg. 2012;5(2):93-103. doi:10.4103/0974-2077.99436
- Prohaska J, Badri T. Cryotherapy. StatPearls Publishing. 2019.
- Schalka S. New data on hyperpigmentation disorders. J Eur Acad Dermatol Venereol. 2017;31 Suppl 5:18-21. doi:10.1111/jdv.14411
- American Academy of Dermatology. Variety of Options Available to Treat Pigmentation Problems. February 5, 2013.
- Tomecki J, Woodhouse G. Common Benign Growths. Cleveland Clinic Center for Continuing Education.
Writer Bio
Dr. Tina M. St. John owns and operates a health communications and consulting firm. She is also an accomplished medical writer and editor, and was formerly a senior medical officer with the U.S. Centers for Disease Control and Prevention. St. John holds an M.D. from Emory University School of Medicine.