Long-Term Effects of Salmonella Poisoning
According to the World Health Organization, salmonella bacteria is one of the most common causes of foodborne illness around the world. In the United States, 1.4 million infections result in over 150,000 doctor visits, 15,000 hospitalizations, and 500 deaths each year. Although salmonella poisoning usually causes mild, self-limited gastroenteritis ("salmonellosis"), in some cases long-term effects may result.
Metastatic Infections
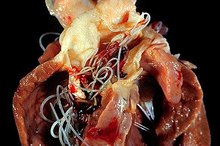
In rare cases, salmonella escapes the intestine to enter the bloodstream. Bloodstream infection may itself be fatal and can produce long-term complications when salmonella spreads (metastasizes) from the bloodstream to infect other areas of the body. Examples of metastatic salmonella infections include infection of the heart valves and lining of the heart (endocarditis), the bone (osteomyelitis), the kidneys (pyelonephritis), and other soft tissues including the brain. Typically, these infections are slow-growing and take much longer to appear than the 12 to 72 hours associated with classic salmonella gastroenteritis. They occur rarely in healthy adults and are much more common in people with compromised immune systems (such as those with AIDS, cancer, sickle cell anemia) or multiple medical problems.
- In rare cases, salmonella escapes the intestine to enter the bloodstream.
- They occur rarely in healthy adults and are much more common in people with compromised immune systems (such as those with AIDS, cancer, sickle cell anemia) or multiple medical problems.
Autoimmune Disease
The After-Effects of the Flu
Learn More
After salmonella exposure, the immune system makes antibodies to the bacteria. Unfortunately, salmonella bacteria resembles a cell surface marker present in many people. The result is an autoimmune disease cause Reiter’s Syndrome, which produces chronic joint pain (arthritis), eye irritation (conjunctivitis with or without iritis) and problems with urination (urethritis). In a 2001 study presented in the journal Clinics in Infectious Disease, nearly one-third of people who were infected with Salmonella Dnteridis, one of the most common salmonella species, developed arthritis that persisted for up to 6 months, and nearly 50 percent reported recurrence after the initial episode resolved.
- After salmonella exposure, the immune system makes antibodies to the bacteria.
- The result is an autoimmune disease cause Reiter’s Syndrome, which produces chronic joint pain (arthritis), eye irritation (conjunctivitis with or without iritis) and problems with urination (urethritis).
Chronic Carriers
In some cases, individuals recover from salmonella infection to become chronic carriers. The most famous example of a human chronic carrier of salmonella is "Typhoid Mary." J.W. Leavitt's 1996 book "Typhoid Mary: Captive to the Public's Health" recounts the true tale of the asymptomatic Irish-American cook linked to 54 cases and four deaths in nine different typhoid fever epidemics in early 1900s New York City.
Nowadays, chronic carrier states can usually be eradicated with an extended course of antibiotics, although individuals may be subject to restrictions on the type of work they may perform in the interim. Most chronic carriers are asymptomatic. However, patients with AIDS and other types of immune compromise may suffer repeated bouts of recurrence before antibiotics are effective.
- In some cases, individuals recover from salmonella infection to become chronic carriers.
- However, patients with AIDS and other types of immune compromise may suffer repeated bouts of recurrence before antibiotics are effective.
Related Articles
References
- Reactive Arthritis and Reiter's Syndrome Following an Outbreak of Gastroenteritis Caused by Salmonella Enteritidis, Clinics in Infectious Disease, October 1, 2001
- Leavitt J.W., Typhoid Mary: Captive to the Public’s Health, 1996
- Salmonella Infection. CDC. https://www.cdc.gov/healthypets/diseases/salmonella.html.
- Salmonella. CDC. https://www.cdc.gov/salmonella/
- Salmonella Outbreak Investigations. CDC. https://www.cdc.gov/salmonella/outbreaks.html.
- Salmonella Questions and Answers. USDA Food Safety and Inspection Service. https://www.fsis.usda.gov/wps/portal/fsis/topics/food-safety-education/get-answers/food-safety-fact-sheets/foodborne-illness-and-disease/salmonella-questions-and-answers.
- Giannella RA. Salmonella. In: Medical Microbiology. 4th ed. Galveston, TX: The University of Texas Medical Branch at Galveston.; 1996.
- Tuompo R, Hannu T, Mattila L, Siitonen A, Leirisalo-repo M. Reactive arthritis following Salmonella infection: a population-based study. Scand J Rheumatol. 2013;42(3):196-202. doi:10.3109/03009742.2012.739201
- Fatica MK, Schneider KR. Salmonella and produce: survival in the plant environment and implications in food safety. Virulence. 2011;2(6):573-9. doi:10.4161/viru.2.6.17880
- Demirbilek SK. Salmonellosis in Animals. Salmonella - A Re-emerging Pathogen. 2018. doi:10.5772/intechopen.72192
- Eng S-K, Pusparajah P, Mutalib N-SA, Ser H-L, Chan K-G, Lee L-H. Salmonella: A review on pathogenesis, epidemiology and antibiotic resistance. Frontiers in Life Science. 2015;8(3):284-293. doi:10.1080/21553769.2015.1051243
- Salmonella Management and Treatment. Cleveland Clinic. Jan 17, 2019.
- Foods Most Likely to Cause Food Poisoning | CDC Food Safety. Centers for Disease Control and Prevention. Aug 4, 2019.
- Four Steps (Clean, Separate, Cook, Chill) to Food Safety | Food Safety | CDC. Centers for Disease Control and Prevention. Jul 21, 2017.
- Prevention | General Information | Salmonella | CDC. Centers for Disease Control and Prevention. Feb 8, 2019.
- Salmonella Infection. CDC.
- Salmonella. CDC.
- Salmonella Outbreak Investigations. CDC.
- Salmonella Questions and Answers. USDA Food Safety and Inspection Service.
Resources
Writer Bio
Heather Gloria began writing professionally in 1990. Her work has appeared in several professional and peer-reviewed publications including "Nutrition in Clinical Practice." Gloria earned both a Bachelor of Science in food science and human nutrition from the University of Illinois. She also maintains the "registered dietitian" credential and her professional interests include therapeutic nutrition, preventive medicine and women's health.