What does fact checked mean?
At Healthfully, we strive to deliver objective content that is accurate and up-to-date. Our team periodically reviews articles in order to ensure content quality. The sources cited below consist of evidence from peer-reviewed journals, prominent medical organizations, academic associations, and government data.
- FDA: Surgical Mesh
- FDA: Counterfeit Polypropylene Surgical Mesh Products Marketed as C. R. Bard/Davol
The information contained on this site is for informational purposes only, and should not be used as a substitute for the advice of a professional health care provider. Please check with the appropriate physician regarding health questions and concerns. Although we strive to deliver accurate and up-to-date information, no guarantee to that effect is made.
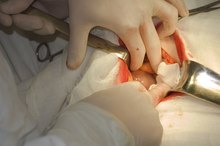
Surgical mesh has been used to help repair all different types of hernias since 1958, according to Dr. Timothy Kuwada, assistant clinical professor of surgery at University of North Carolina. Even though surgical mesh helps hernias to heal faster and with less pain than just closing a hernia, allergic reactions, complications and recurrence rates still abound.
If you are experiencing serious medical symptoms, seek emergency treatment immediately.
Dr. Yuri Novitsky, director of the Hernia Center at the University of Connecticut Health Center, explains that the ideal synthetic mesh has to be durable and strong and not contract within human tissue. It has to be hypoallergenic, noncarcinogenic and resistant to infection. It must be absorbed into body tissue without causing excessive inflammation or immune response and it has to be cost-effective.
Surgical Mesh Complications
Kuwada reports that infections and fistulas (abnormal holes) resulting from surgical mesh can be devastating. Research suggests that surgical mesh may increase chronic pain and discomfort as it inflames nerves and tissues and feels rigid and unnatural.
The body recognizes that the material isn’t organic and rejection and allergic reactions arise. The FDA also reports that the use of surgical mesh can result in adhesions of organs, injuries to nearby organs and damage to blood vessels and nerves.
- Kuwada reports that infections and fistulas (abnormal holes) resulting from surgical mesh can be devastating.
- The FDA also reports that the use of surgical mesh can result in adhesions of organs, injuries to nearby organs and damage to blood vessels and nerves.
Heavyweight Mesh Versus Lightweight Mesh
Post Operative Complications of Abdominal-Hernia Surgery
Learn More
Heavyweight mesh is made of heavier and sturdier material than the newer lightweight meshes. Because lightweight meshes contain less foreign material, it is thought that they may inspire less allergic and inflammatory reactions and less pain and contraction.
Lightweight mesh, however, isn’t as strong as heavyweight mesh and hernia recurrence rates may be higher with its use.
Novitsky says that even though evidence exists that lightweight mesh may give mild-to-moderate pain reduction in groin hernia repair, not enough evidence exists to state that it is better than heavyweight mesh.
- Heavyweight mesh is made of heavier and sturdier material than the newer lightweight meshes.
- Lightweight mesh, however, isn’t as strong as heavyweight mesh and hernia recurrence rates may be higher with its use.
Synthetic Surgical Mesh
Dr. Bruce Ramshaw, chief of surgery at the University of Missouri, explains that in current practice, either woven mesh or nonwoven mesh is used. Woven mesh has large pores and comes in a variety of weaves. It is made of polypropylene, which has been compared to polyester.
Nonwoven mesh is made of a Teflon derivative known as ePTFE. Because it is microporous, it minimizes the ingrowth of tissue.
These synthetic materials are the least expensive surgical meshes. Biomeshes currently are the most expensive choice, but Ramshaw reports that research of a new class of "nano" meshes embedded with growth factors and inflammation inhibitors is under way.
- Dr. Bruce Ramshaw, chief of surgery at the University of Missouri, explains that in current practice, either woven mesh or nonwoven mesh is used.
- Biomeshes currently are the most expensive choice, but Ramshaw reports that research of a new class of "nano" meshes embedded with growth factors and inflammation inhibitors is under way.
Biologic Mesh
Types of Surgical Glue
Learn More
Biomeshes, surgical mesh made of human or other animal skin cells, were first developed in the 1990s for use in burn recovery.
Since then, biomeshes have been developed for use in hernia and abdominal wall reconstruction. Dr. Scott Helton, chairman of surgery at the Hospital of St. Raphael in New Haven, reports that 13 biomeshes had been as of 2008. He also reports that six of those products have never undergone valid clinical study.
Biomeshes are very expensive, but Helton believes the cost is balanced by the advantages: Biomesh is less likely to lead to fistulas, it speeds healing, it is more resistant to infection and may be more absorbable.
Not enough is known about biomesh strength and hernia recurrence with their use. There is worry over viral infections carried in the animal tissue used and medical and legal issues concerning the implantation of animal tissue into humans.
- Biomeshes, surgical mesh made of human or other animal skin cells, were first developed in the 1990s for use in burn recovery.
- Since then, biomeshes have been developed for use in hernia and abdominal wall reconstruction.
Surgical Mesh for Pelvic Organ Prolapse and Stress Urinary Incontinence
The FDA has received over 1,000 reports from nine different surgical mesh manufacturers about complications when mesh is put in place through an incision in the wall of the vagina.
Used to treat pelvic organ prolapse and stress urinary incontinence, this surgical mesh procedure has led to abcesses, infections, pain, urinary problems, erosion of the mesh into the vagina and vaginal scarring. Blood vessel, bladder and bowel injury have also occurred.
The complications have not yet been linked to any one type or brand of surgical mesh.
- The FDA has received over 1,000 reports from nine different surgical mesh manufacturers about complications when mesh is put in place through an incision in the wall of the vagina.
Recall of Kugel Mesh
**The most widely used hernia repair patches.
** Kugel mesh hernia patches were manufactured by Davol Inc.
Patients who received Kugel mesh experienced reactions to the materials and breakdown of the product. The breakage has perforated patient bowels and obstructed bowels.
Several patches have been recalled since 2005, reports the website "Drug Recall Side Effects News," including Bard and Composix.
- The most widely used hernia repair patches.
- Kugel mesh hernia patches were manufactured by Davol Inc.
- Patients who received Kugel mesh experienced reactions to the materials and breakdown of the product.
Other Surgical Mesh Recalls
The FDA has recalled a counterfeit surgical mesh illegally manufactured and distributed under the C.R. Bard/Davol brand name from Oct. 21, 2008, to Oct. 27, 2009. The product does not meet the Bard/Davol specifications for manufacture and they were not produced by that company.
Surgical mesh with the brand name "Proceed" was the focus of a recall issued by the FDA in December 2005 1. This mesh delaminates and exposes the bowel to the polypropylene, increasing risk of organ adhesions and fistulas.
Shelhigh Inc. has been making implantable medical devices, including surgical mesh, since 1997. The FDA ordered a seizure of all Shelhigh implantable devices in 2007 because they may have been manufactured under contaminated conditions.
- The FDA has recalled a counterfeit surgical mesh illegally manufactured and distributed under the C.R.
- Bard/Davol brand name from Oct. 21, 2008, to Oct. 27, 2009.
- The FDA ordered a seizure of all Shelhigh implantable devices in 2007 because they may have been manufactured under contaminated conditions.
Related Articles
References
Writer Bio
Sumei FitzGerald has been writing professionally since 2008 on health, nutrition, medicine and science topics. She has published work on doctors' websites such as Colon Cancer Resource, psychology sites such as Webpsykologen and environmental websites such as Supergreenme. She holds a Bachelor of Arts in sociology from the University of Connecticut where she also studied life sciences.