What does fact checked mean?
At Healthfully, we strive to deliver objective content that is accurate and up-to-date. Our team periodically reviews articles in order to ensure content quality. The sources cited below consist of evidence from peer-reviewed journals, prominent medical organizations, academic associations, and government data.
The information contained on this site is for informational purposes only, and should not be used as a substitute for the advice of a professional health care provider. Please check with the appropriate physician regarding health questions and concerns. Although we strive to deliver accurate and up-to-date information, no guarantee to that effect is made.
Fissures & Athlete's Feet Treatment
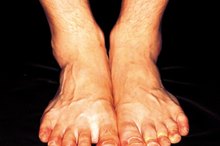
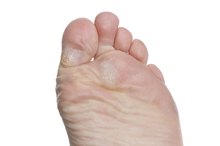
Many people experience dry, cracking skin on their feet, but painful or inflamed cracks may rightfully cause concern. Deep cracks on the heel, called heel fissures, can lead to further complications. Cracks or fissures between the toes could be a sign of athlete's foot, a common foot infection. If you're concerned, contact your doctor, especially if you have bleeding or pussy fissures.
Understanding the Cause
Heel fissures occur when pressure cracks apart the hard skin of the heel. The likelihood of fissures increases if the skin is dehydrated, making it even more inflexible. A bacteria or fungus does not directly cause the condition, but if left untreated, an infection could develop.
Skin fissures due to athlete's foot typically result from fungal infection; though, bacterial infections and chronic skin conditions may also factor in. Athlete's foot spreads through contact with infected skin scales or fungi found in damp areas, such as swimming pools or locker rooms, according to the Centers for Disease Control and Prevention 2.
- Heel fissures occur when pressure cracks apart the hard skin of the heel.
- A bacteria or fungus does not directly cause the condition, but if left untreated, an infection could develop.
Preventative Treatment
The Skin on My Big Toe Is Peeling
Learn More
To prevent fissures and athlete's foot, avoid walking around barefoot 2. Walking barefoot causes friction, hardening the skin of the heel. Walking barefoot in damp areas also puts you at risk for catching fungi responsible for athlete's foot. Wearing sandals around pools and shared showers reduces this risk. The Harvard Medical School Family Health Guide also notes that you should regularly wash your feet with soap and water, but should otherwise keep them dry. If you suffer from unusually sweaty feet, foot powders may help dry them out. People with excessively dry feet should apply specially formulated foot moisturizers to prevent heel fissures.
- To prevent fissures and athlete's foot, avoid walking around barefoot 2.
- The Harvard Medical School Family Health Guide also notes that you should regularly wash your feet with soap and water, but should otherwise keep them dry.
Home Treatment
Once heel fissures develop, use deep skin moisturizers to hydrate and heal the damaged skin. If you have excessive dry skin around the heels, remove any dead skin with a foot file or pumice soap.
Manage the early stages of athlete's foot with home treatment. Regular foot washing and thorough drying prevents the infection from worsening. Focus on keeping your feet as dry as possible, especially around the toe area, where athlete's foot generally settles. Over-the-counter anti-fungal creams also help reduce the amount of fungi.
- Once heel fissures develop, use deep skin moisturizers to hydrate and heal the damaged skin.
- If you have excessive dry skin around the heels, remove any dead skin with a foot file or pumice soap.
Professional Medical Treatment
How to Treat Cracked Diabetic Feet
Learn More
If heel fissures break into open wounds, seek professional medical treatment to reduce the risk of infection. Professional treatment may include the removal of the callus, an intense moisturizing regiment or a prescription medication to fight off any possible infection.
If you've suffered from athlete's foot for more than two weeks or if the infection results in blistering fissures, consult a doctor. A doctor may either prescribe an oral anti-fungal or a topical medication such as clotrimazole and miconazole. The doctor will provide professional advice for easing painful symptoms and may also prescribe an oral antibiotic if a bacterial infection presents itself.
- If heel fissures break into open wounds, seek professional medical treatment to reduce the risk of infection.
- Professional treatment may include the removal of the callus, an intense moisturizing regiment or a prescription medication to fight off any possible infection.
Related Articles
References
- New Zealand Dermatological Society Incorporated: Athlete's Foot
- Centers for Disease Control and Prevention: Athlete's Foot
- Homei A, Worboys M. Fungal Disease in Britain and the United States 1850–2000: Mycoses and Modernity. Basingstoke (UK): Palgrave Macmillan; 2013. Chapter 2, Athlete’s Foot: A Disease of Fitness and Hygiene. Available from: https://www.ncbi.nlm.nih.gov/books/NBK169220/
- InformedHealth.org [Internet]. Cologne, Germany: Institute for Quality and Efficiency in Health Care (IQWiG); 2006-. Nail fungus: Overview. 2015 Jan 14 [Updated 2018 Jun 14].Available from: https://www.ncbi.nlm.nih.gov/books/NBK279547/
- InformedHealth.org [Internet]. Cologne, Germany: Institute for Quality and Efficiency in Health Care (IQWiG); 2006-. Athlete's foot: Overview. 2015 Jan 14 [Updated 2018 Jun 14].Available from: https://www.ncbi.nlm.nih.gov/books/NBK279549/
- Nigam PK, Saleh D. Tinea Pedis. [Updated 2019 Nov 25]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK470421/
- Abd Elmegeed AS, Ouf SA, Moussa TA, Eltahlawi SM. Dermatophytes and other associated fungi in patients attending to some hospitals in Egypt. Braz J Microbiol. 2015;46(3):799–805. doi:10.1590/S1517-838246320140615
- Homei A, Worboys M. Fungal Disease in Britain and the United States 1850–2000: Mycoses and Modernity. Basingstoke (UK): Palgrave Macmillan; 2013. Chapter 2, Athlete’s Foot: A Disease of Fitness and Hygiene.
- InformedHealth.org [Internet]. Cologne, Germany: Institute for Quality and Efficiency in Health Care (IQWiG); 2006-. Nail fungus: Overview. 2015 Jan 14 [Updated 2018 Jun 14].
- InformedHealth.org [Internet]. Cologne, Germany: Institute for Quality and Efficiency in Health Care (IQWiG); 2006-. Athlete's foot: Overview. 2015 Jan 14 [Updated 2018 Jun 14].
- Nigam PK, Saleh D. Tinea Pedis. [Updated 2019 Nov 25]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-.
- Leyden JJ, Kligman AM. Interdigital athlete's foot: new concepts in pathogenesis. Postgrad Med. 1977;61(6):113-6.
- Blutfield MS, Lohre JM, Pawich DA, Vlahovic TC. The Immunologic Response to Trichophyton Rubrum in Lower Extremity Fungal Infections. J Fungi (Basel). 2015;1(2):130–137. doi:10.3390/jof1020130
- Al Hasan M, Fitzgerald SM, Saoudian M, Krishnaswamy G. Dermatology for the practicing allergist: Tinea pedis and its complications. Clin Mol Allergy. 2004;2(1):5. Published 2004 Mar 29. doi:10.1186/1476-7961-2-5
- Chollet A, Cattin V, Fratti M, Mignon B, Monod M. Which Fungus Originally was Trichophyton mentagrophytes? Historical Review and Illustration by a Clinical Case. Mycopathologia. 2015;180(1-2):1-5. doi:10.1007/s11046-015-9893-2
- Newland JG, Abdel-Rahman SM. Update on terbinafine with a focus on dermatophytoses. Clin Cosmet Investig Dermatol. 2009;2:49–63. Published 2009 Apr 21. doi:10.2147/ccid.s3690
- Hainer BL. Dermatophyte infections. Am Fam Physician. 2003;67(1):101-8.
- Jimenez-garcia L, Celis-aguilar E, Díaz-pavón G, et al. Efficacy of topical clotrimazole vs. topical tolnaftate in the treatment of otomycosis. A randomized controlled clinical trial. Braz J Otorhinolaryngol. 2019.
- Lestner J, Hope WW. Itraconazole: an update on pharmacology and clinical use for treatment of invasive and allergic fungal infections. Expert Opin Drug Metab Toxicol. 2013;9(7):911-26.
Writer Bio
Caitlynn Lowe has been writing since 2006 and has been a contributing writer for Huntington University's "Mnemosyne" and "Huntingtonian." Her writing has also been in "Ictus" and "Struggle Creek: A Novel Story." Lowe earned her Bachelor of Arts degree in English from Huntington University.