Causes for Blood Count to Drop
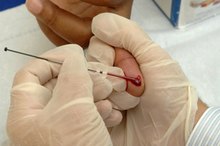
Blood is made of three types of cells that are produced inside the bones: white blood cells fight infections; red blood cells provide energy and carry oxygen to different organs; and platelets thicken the blood so that it clots during injury. A complete blood count is performed to determine abnormalities in the different types of blood cells in order to intervene with the appropriate medical treatment. Each kind of blood cell count can drop due to different factors such as medications or medical conditions.
Myelofibrosis and Leukemia
Myelofibrosis is a serious bone marrow disorder that causes a drop in red blood count and disrupts the normal production of blood cells, according to MayoClinic.com. This condition develops when the stem cells in the blood mutate and replicate. The result of mutation is low red blood cells, which causes an overproduction of white blood cells. Myelofibrosis can occur any time, though it is more common in people over the age of 50. Myelofibrosis can lead to leukemia, a form of cancer impacting blood formation and bone marrow.
- Myelofibrosis is a serious bone marrow disorder that causes a drop in red blood count and disrupts the normal production of blood cells, according to MayoClinic.com.
- Myelofibrosis can lead to leukemia, a form of cancer impacting blood formation and bone marrow.
Anemia
What Are the Causes of Low Platelets & Low White Blood Cells?
Learn More
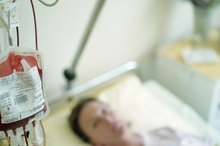
Anemia is a drop in red blood cells. Megaloblastic anemia is a rare form of anemia in which red blood cells are deficient due to digestive disturbance in absorbing vitamin B12. The University of Maryland Medical Center notes that treatment for this condition includes increasing intake of foods rich in folic acid or B12, and injections to stimulate red blood cell production. Aplastic anemia is another form of anemia that impacts all three blood cell types. This condition causes hemoglobin, oxygenated protein in the red blood cells, to drop as well as increases susceptibility to infections due to a low white blood count. In the event of aplastic anemia, a blood transfusion is a plausible treatment for increasing red blood cells and platelets.
- Anemia is a drop in red blood cells.
- Megaloblastic anemia is a rare form of anemia in which red blood cells are deficient due to digestive disturbance in absorbing vitamin B12.
Chemotherapy
Chemotherapy is intended to treat certain cancers; however, chemotherapy medications also cause the white blood cell count to drop, notes Pfizer Oncology. In most conditions requiring chemotherapy, the white blood count is too high, thus indicating a need for treatment. Once treatment is completed, white blood count returns to normal levels. Chemotherapy can also cause a drop in red blood cell count due to increasing the risk of anemia. Medications for aiding the body to produce red blood cells during chemotherapy are available.
- Chemotherapy is intended to treat certain cancers; however, chemotherapy medications also cause the white blood cell count to drop, notes Pfizer Oncology.
Medications
What Are the Causes of Low Platelets & Low White Blood Cells?
Learn More
According to MayoClinic.com, certain medications can cause a thrombocytopenic reaction. Thrombocytopenia is when blood platelet count is low. Medications contributing to low platelets include sulfa-containing antibiotics, antiarrhythmic medications used for treating abnormal heart rhythms and anticoagulants which treat blood clots in the veins. Once medications are ceased, platelet counts can return to normal.
- According to MayoClinic.com, certain medications can cause a thrombocytopenic reaction.
- Medications contributing to low platelets include sulfa-containing antibiotics, antiarrhythmic medications used for treating abnormal heart rhythms and anticoagulants which treat blood clots in the veins.
Related Articles
References
- MedlinePlus: CBC
- Mayo Clinic: Low White Blood Cell Count
- Auerbach M, Adamson JW. How we diagnose and treat iron deficiency anemia. Am J Hematol. 2016;91(1):31-38. doi:10.1002/ajh.24201
- Penn State Hersey. Milton S. Hersey Medical Center. CBC Blood Test. Updated October 24, 2018.
- Whitehead L. Managing Chemotherapy-Induced Anemia with Erythropoiesis-Stimulating Agents Plus Iron. Am J Nurs. 2017;117(5):67. doi:10.1097/01.NAJ.0000516277.58981.36
- Mohandas H, Jaganathan SK, Mani MP, Ayyar M, Rohini Thevi GV. Cancer-related fatigue treatment: An overview. J Cancer Res Ther. 2017;13(6):916-929. doi:10.4103/jcrt.JCRT_50_17
- Long B, Koyfman A. Oncologic Emergencies: The Fever With Too Few Neutrophils. J Emerg Med. 2019;57(5):689-700. doi:10.1016/j.jemermed.2019.08.009
- Bond TC, Szabo E, Gabriel S, et al. Meta-analysis and indirect treatment comparison of lipegfilgrastim with pegfilgrastim and filgrastim for the reduction of chemotherapy-induced neutropenia-related events. J Oncol Pharm Pract. 2018;24(6):412-423. doi:10.1177/1078155217714859
- National Heart, Lung, and Blood Institute. Thrombocytopenia. 2019.
- Kuter DJ. Managing thrombocytopenia associated with cancer chemotherapy. Oncology (Williston Park). 2015;29(4):282-294.
- Sunkesula VC, Knighton S, Zabarsky TF, Kundrapu S, Higgins PA, Donskey CJ. Four Moments for Patient Hand Hygiene: A Patient-Centered, Provider-Facilitated Model to Improve Patient Hand Hygiene. Infect Control Hosp Epidemiol. 2015;36(8):986-989. doi:10.1017/ice.2015.78
Resources
Writer Bio
Aubri John has been a contributing researcher and writer to online physical and mental health oriented journals since 2005. John publishes online health and fitness articles that coincide with her licensed clinical skills in addictions, psychology and medical care. She has a master's degree in clinical social work and a Ph.D. in health psychology.