What does fact checked mean?
At Healthfully, we strive to deliver objective content that is accurate and up-to-date. Our team periodically reviews articles in order to ensure content quality. The sources cited below consist of evidence from peer-reviewed journals, prominent medical organizations, academic associations, and government data.
The information contained on this site is for informational purposes only, and should not be used as a substitute for the advice of a professional health care provider. Please check with the appropriate physician regarding health questions and concerns. Although we strive to deliver accurate and up-to-date information, no guarantee to that effect is made.
How to Put in a Coude Catheter
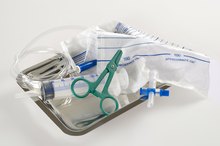
Catheters are used for a wide variety of medical issues in many areas of the body. The most common use for catheters is for urine collection and to provide access to the bladder. Occasionally, difficulty can be encountered with insertion of a traditional "foley" catheter due to issues such as an enlarged prostate gland in males, or unusually small urethral opening and/or strictures within the urethra (channel from the bladder to the outside) in both sexes. When these situations arise, there is a type of catheter that can be used which can provide increased ease of use and a less traumatic means of inserting a catheter in a difficult situation: the Coude catheter.
Select the appropriate size catheter. In adults, the most common size foley urine catheter used is the #18fr. Somewhat less common is the #16fr. When selecting a Coude catheter, keeping in mind it is being used for some type of problem situation, it is common practice to select one that is anywhere from one to three sizes smaller. The goal is to insert the catheter without causing damage to the urethra and to navigate any potential obstruction, so if you have to go smaller, go smaller. Sizes of Coude catheters frequently used range from #14 down to #12 to replace a #18 foley.
How to Irrigate or Flush a Catheter
Learn More
Check the balloon located near the tip of the catheter, which is what helps keep the catheter in the bladder, and make sure it is fully functional and capable of holding the required amount of fluid used to inflate it (approx. 10 cc).
Place lubrication at the tip of the catheter while both hands are still sterile, so that it is ready to go and easily handled by one hand. Most catheterization kits come with a packet of lubricating gel inside. Occasionally it may be necessary to use a lubricating gel that has a local anesthetic incorporated into it. This is typically obtained from a source other than the kit. If connecting to a collection system, have that done ahead of time. If simply using the catheter to collect a urine specimen, have a sterile specimen container readily available and near the work area.
How to Remove a Catheter
Learn More
Place the necessary sterile drapes around the site Io be cleansed prior to insertion. When catheterizing, one hand will become contaminated because of holding the penis or labia for the procedure. Make sure all equipment and supplies are readily accessible with the sterile hand.
Cleanse the urethra. In males the tip of the penis should be cleansed with an appropriate solution such as Betadine or Chlorhexadine. In females the urethral opening and inner labia should be cleansed, beginning at the urethral opening and swiping to the rear toward the anus. Repeat this process with a new swab each time to avoid cross-contamination.
Lubricate the tip of the catheter and slowly begin to insert it into the urethral opening. With a Coude catheter, you should keep the angled tip facing in the direction of the front of the patient. This ensures that the catheter will follow the natural curvature of the urethra. The catheter should slide relatively smoothly. Encountering some minimal resistance is not uncommon, but if there is a total blockage or significant pressure is required, you should abort the procedure and consult a physician.
Make sure the catheter has reached the bladder 1. In females you only have to insert the catheter approximately one to two inches to access the bladder; in males, approximately four inches. Additionally, in males there will be a slight resistance when the tip of the catheter encounters the opening through the prostate, but should pass with minimal pressure. Once past this landmark, you should be in the bladder. In females the only major sign of being in the bladder will be a return of urine.
Inflate the balloon. Once you have verified that you are in the bladder, proceed with inflation of the balloon with the appropriate amount of saline fluid using the accompanying, pre-filled syringe. Then, gently pull back on the catheter until it stops. This demonstrates that the balloon is properly inflated and preventing the catheter from slipping out of the bladder.
Tips
Be sure to maintain sterility when inserting catheter Gently positioning the penis in an upward inclination improves ease of catheter insertion Be sure Coude catheter is not too big Keep tip of Coude catheter facing the front of the body during insertion
Warnings
Never force catheter into the urethra or through prostate opening into bladder Do not inflate balloon until placement is verified by a return of urine Verify placement of balloon and catheter by gently pulling back until it stops
Related Articles
References
- Medicine Plus; Urinary Catheters
- Håkansson MÅ. Reuse versus single-use catheters for intermittent catheterization: what is safe and preferred? Review of current status. Spinal Cord. 2014;52(7):511-6. doi:10.1038/sc.2014.79
- National Clinical Guideline Centre (UK), Royal College of Physicians (UK). Long term urinary catheters. In: Infection: prevention and control of healthcare-associated infections in primary and community care. London: National Clinical Guideline Centre, 2012.
- Willette PA, Coffield S. Current trends in the management of difficult urinary catheterizations. West J Emerg Med. 2012;13(6):472-8. doi:10.5811/westjem.2011.11.6810
- Cortese YJ, Wagner VE, Tierney M, Devine D, Fogarty A. Review of catheter-associated urinary tract infections and urinary tract models. J Healthc Eng. 2018;2018:2986742. doi:10.1155/2018/2986742
- Urinary catheter types and being part of the insertion team. Agency for Healthcare Research and Quality. Updated April 2017.
- Guide to implementing a program to reduce catheter-associated urinary tract infections in long-term care. Agency for Healthcare Research and Quality. Published March 2017.
- Urinary Catheters. Medline Plus. Updated January 6, 2020.
- Infection control: catheter-associated urinary tract infections. Summary of recommendations. Centers for Disease Control and Prevention. Updated November 5, 2015.
- Feneley RC, Hopley IB, Wells PN. Urinary catheters: history, current status, adverse events and research agenda [published correction appears in J Med Eng Technol. 2016;40(2):59]. J Med Eng Technol. 2015;39(8):459–470. doi:10.3109/03091902.2015.1085600
- Meddings J, Saint S, Fowler KE, et al. The Ann Arbor criteria for appropriate urinary catheter use in hospitalized medical patients: results obtained by using the RAND/UCLA appropriateness method. Ann Intern Med. 2015;162(9 Suppl):S1-34. doi:10.7326/M14-1304
Tips
- Be sure to maintain sterility when inserting catheter Gently positioning the penis in an upward inclination improves ease of catheter insertion Be sure Coude catheter is not too big Keep tip of Coude catheter facing the front of the body during insertion
Warnings
- Never force catheter into the urethra or through prostate opening into bladder Do not inflate balloon until placement is verified by a return of urine Verify placement of balloon and catheter by gently pulling back until it stops
Writer Bio
Ken Chisholm is a freelance writer who began writing in 2007 for LIVESTRONG.COM. He has experience in health care, surgery, nursing and orthopedics as an orthopedic physician assistant and a registered nurse. He holds a bachelor's degree in business from the University of Findlay, Ohio.