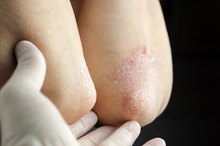
Melasma in Kids
Melasma is a disorder that causes parts of the skin to become dark brown. Although melasma is purely a superficial skin condition--it is not related in any way to cancer or any other serious health problem--it can be difficult for affected individuals to deal with the uneven and patchy coloring of their skin. Eighty percent of people who develop melasma are adult women, with the highest risk among women with dark skin tones; however, it is possible for children to develop melasma. As a parent, there are a number of preventative measures you can take to help decrease the chance of your child developing melasma as he gets older.
Causes
According to the Mayo Clinic and the American Academy of Dermatology, melasma has four main causes: excessive exposure to the ultraviolet rays in sunlight; a high circulating blood concentration of the hormones estrogen and progesterone; the inheritance of a predisposition for the disorder; and a skin-care product that irritates the skin and results in an excessive production of melanocytes, the skin's pigment-producing cells. While most of these causes do not generally result in children developing melasma, their effects can, over time, accumulate to make children more susceptible later in life. Because of the strong link between the female hormones estrogen and progesterone and melasma, women who are experiencing an upsurge in these hormones due to hormone-replacement therapy in menopause, pregnancy or from birth control pills have a greater tendency to develop melasma. Additionally, certain cosmetics and medications, such as many anti-seizure medications, can make the skin more sensitive to the effects of ultraviolet light.
- According to the Mayo Clinic and the American Academy of Dermatology, melasma has four main causes: excessive exposure to the ultraviolet rays in sunlight; a high circulating blood concentration of the hormones estrogen and progesterone; the inheritance of a predisposition for the disorder; and a skin-care product that irritates the skin and results in an excessive production of melanocytes, the skin's pigment-producing cells.
Symptoms
Hyperpigmentation While on Birth Control
Learn More
Melasma causes symmetrical splotches of dark brown, gray, bluish, black or tan pigmented skin to develop anywhere that the skin receives a lot of exposure to the sun, especially the cheeks, chin, forehead, nose, neck and arms.cause:
- Melasma causes symmetrical splotches of dark brown
- gray
- bluish
- black or tan pigmented skin to develop anywhere that the skin receives a lot of exposure to the sun
- especially the cheeks
- chin
- forehead
- nose
- neck
- arms
There are no other systemic symptoms associated with melasma.
Diagnosis
Melasma is most often diagnosed through a dermatological examination. However, the American Academy of Dermatology reports that many doctors will conduct a small skin biopsy to test the skin's epithelial cells and confirm that the discoloration is due to melasma. A physician may also use a Wood's lamp to aid in the diagnosis. A Wood's lamp is a special ultraviolet light used in a dark room that is capable of illuminating portions of skin that have changed color, even when those pigmentation changes are invisible to the eye.
- Melasma is most often diagnosed through a dermatological examination.
- However, the American Academy of Dermatology reports that many doctors will conduct a small skin biopsy to test the skin's epithelial cells and confirm that the discoloration is due to melasma.
Treatment
Treatments for Melasma in Males
Learn More
The American Academy of Dermatology reports that, in many cases, the patches caused by melasma vanish on their own, especially if they were originally caused by the hormonal fluctuations due to birth control pills or pregnancy. However, there are a variety of treatments for cases in children for symptoms that do not resolve on their own. Dermanetwork.org notes that these treatments can include chemical peels, laser resurfacing, bleaching creams and intense pulsed light therapy, a type of treatment that uses strong broadband light to decrease skin discoloration 1.
Prevention
According to Joiedevie.com, nearly 80 percent of the sun damage your skin will sustain in your lifetime occurs within your first 18 years of life. It can take several decades for this damage to manifest itself as melasma. The best way to reduce your child's risk of melasma, as well as your own, is to use sunscreen regularly and consistently and to stay out of direct sunlight as much as possible. According to the Mayo Clinic, you should use a daily sunscreen with UVA and UVB protection that also features an SPF of more than 30, even when you are mainly within a building and not in direct sunlight. When you are going to spend time outdoors, use a sunscreen with an SPF greater than 45. Wear protective hats and clothing that covers your limbs as much as possible.
- According to Joiedevie.com, nearly 80 percent of the sun damage your skin will sustain in your lifetime occurs within your first 18 years of life.
- According to the Mayo Clinic, you should use a daily sunscreen with UVA and UVB protection that also features an SPF of more than 30, even when you are mainly within a building and not in direct sunlight.
Related Articles
References
- Dermanetwork.org: Melasma
- Joiedevie.com: About Hyper-Pigmentation
- Achar A, Rathi SK. Melasma: a clinico-epidemiological study of 312 cases. Indian J Dermatol. 2011;56(4):380-382. doi:10.4103/0019-5154.84722
- Handel AC, Miot LDB, Miot HA. Melasma: a clinical and epidemiological review. An Bras Dermatol. 2014;89(5):771-782. doi:10.1590/abd1806-4841.20143063
- Plensdorf S, Martinez J. Common pigmentation disorders. Am Fam Physician. 2009;79(2):109-116.
- Cestari TF, Dantas LP, Boza JC. Acquired hyperpigmentations. An Bras Dermatol. 2014;89(1):11-25. doi:10.1590/abd1806-4841.20142353
- Yamaguchi Y, Hearing VJ. Melanocytes and their diseases. Cold Spring Harb Perspect Med. 2014;4(5). doi:10.1101/cshperspect.a017046
- Ogbechie-Godec OA, Elbuluk N. Melasma: an Up-to-Date Comprehensive Review. Dermatol Ther. 2017;7(3):305-318. doi:10.1007/s13555-017-0194-1
- Basit H, Godse KV, Al Aboud AM. Melasma. In: StatPearls. Treasure Island, FL: StatPearls Publishing; 2019.
- Pichardo R, Vallejos Q, Feldman SR, et al. The prevalence of melasma and its association with quality of life in adult male Latino migrant workers. Int J Dermatol. 2009;48(1):22-26. doi:10.1111/j.1365-4632.2009.03778.x
- Sarkar R, Ailawadi P, Garg S. Melasma in Men: A Review of Clinical, Etiological, and Management Issues. J Clin Aesthet Dermatol. 2018;11(2):53-59.
- Passeron T, Picardo M. Melasma, a photoaging disorder. Pigment Cell Melanoma Res. 2018;31(4):461-465. doi:10.1111/pcmr.12684
- Rivas S, Pandya AG. Treatment of melasma with topical agents, peels and lasers: an evidence-based review. Am J Clin Dermatol. 2013;14(5):359-376. doi:10.1007/s40257-013-0038-4
- Jadotte YT, Schwartz RA. Melasma: insights and perspectives. Acta Dermatovenerol Croat. 2010;18(2):124-129.
- Vashi NA, Kundu RV. Facial hyperpigmentation: causes and treatment. Br J Dermatol. 2013;169 Suppl 3:41-56. doi:10.1111/bjd.12536
- Hasegawa K, Fujiwara R, Sato K, et al. Possible Involvement of Keratinocyte Growth Factor in the Persistence of Hyperpigmentation in both Human Facial Solar Lentigines and Melasma. Ann Dermatol. 2015;27(5):626-629. doi:10.5021/ad.2015.27.5.626
- Plensdorf S, Livieratos M, Dada N. Pigmentation Disorders: Diagnosis and Management. Am Fam Physician. 2017;96(12):797-804.
- Shankar K, Godse K, Aurangabadkar S, et al. Evidence-based treatment for melasma: expert opinion and a review. Dermatol Ther. 2014;4(2):165-186. doi:10.1007/s13555-014-0064-z
- Grimes PE, Ijaz S, Nashawati R, Kwak D. New oral and topical approaches for the treatment of melasma. Int J Womens Dermatol. 2019;5(1):30-36. doi:10.1016/j.ijwd.2018.09.004
- Handa S, De D, Khullar G, Radotra BD, Sachdeva N. The clinicoaetiological, hormonal and histopathological characteristics of melasma in men. Clin Exp Dermatol. 2018;43(1):36-41. doi:10.1111/ced.13234
- Lee A-Y. Recent progress in melasma pathogenesis. Pigment Cell Melanoma Res. 2015;28(6):648-660. doi:10.1111/pcmr.12404
Writer Bio
Michelle Kerns writes for a variety of print and online publications and specializes in literature and science topics. She has served as a book columnist since 2008 and is a member of the National Book Critics Circle. Kerns studied English literature and neurology at UC Davis.