What does fact checked mean?
At Healthfully, we strive to deliver objective content that is accurate and up-to-date. Our team periodically reviews articles in order to ensure content quality. The sources cited below consist of evidence from peer-reviewed journals, prominent medical organizations, academic associations, and government data.
The information contained on this site is for informational purposes only, and should not be used as a substitute for the advice of a professional health care provider. Please check with the appropriate physician regarding health questions and concerns. Although we strive to deliver accurate and up-to-date information, no guarantee to that effect is made.
Skin Fungus That Causes White Spots
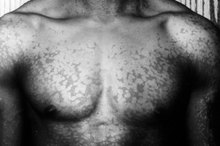
Just the idea of any kind of skin fungus is enough to make you feel itchy and uncomfortable. However, everybody has fungi and bacteria that naturally occurs on the skin. When a certain type of fungus starts to grow rapidly, it causes a condition known as tinea versicolor. This fungal infection disables the cells that cause the skin to tan, so areas of the skin that are infected will often appear as white spots or patches.
Causes
Tinea versicolor is a fungal infection of the skin caused by the yeast Pityrosporum ovale. According to the National Institutes of Health, this yeast occurs naturally on everyone's skin. When the yeast starts to multiply rapidly, it can form small colonies on the skin's surface. The reason the yeast does this on some people but not others is unknown, but it is known that tinea versicolor is not contagious. It is most likely to occur during hot weather, presumably because increased moisture on the skin through sweating creates an environment that encourages fungal growth.
- Tinea versicolor is a fungal infection of the skin caused by the yeast Pityrosporum ovale.
- It is most likely to occur during hot weather, presumably because increased moisture on the skin through sweating creates an environment that encourages fungal growth.
Identification
Stages of Tinea Versicolor
Learn More
The patches caused by tinea versicolor can vary in appearance. When a person is exposed to sun and his skin tans, areas affected by tinea versicolor will appear as white spots or patches. The patches can also appear as pink or red spots on untanned skin, and when the infection has been left for a long while, the patches can appear to be a pinkish brown color. You also may notice very slight flaking on the patches upon close examination. Most doctors will diagnose tinea versicolor based upon a visual inspection of the affected areas, but a skin scraping examined under a microscope also can be used for diagnosis.
- The patches caused by tinea versicolor can vary in appearance.
- When a person is exposed to sun and his skin tans, areas affected by tinea versicolor will appear as white spots or patches.
Treatment
Because this infection is on the surface of the skin, topical applications are used to treat it. These antifungal medications can be over the counter or prescribed by a doctor in greater strength. According to the National Institutes of Health, applying dandruff shampoo to the affected area and allowing it to sit for 10 minutes before rinsing also can treat tinea versicolor 1. This treatment would need to be applied for several days, up to two weeks, before resolution occurs.
- Because this infection is on the surface of the skin, topical applications are used to treat it.
- According to the National Institutes of Health, applying dandruff shampoo to the affected area and allowing it to sit for 10 minutes before rinsing also can treat tinea versicolor 1.
Prevention
Skin Problems That Cause Eyebrow Loss
Learn More
According to the National Institutes of Health, tinea versicolor is a chronic condition 1. This means that it is likely to reoccur on someone who has experienced this type of infection. The National Institute of Health recommends that people prone to this type of infection should avoid excessive sweating. Some people also find that, once an outbreak has been treated and has cleared up, using a dandruff shampoo once per week to wash the body while bathing can prevent future outbreaks.
- According to the National Institutes of Health, tinea versicolor is a chronic condition 1.
- Some people also find that, once an outbreak has been treated and has cleared up, using a dandruff shampoo once per week to wash the body while bathing can prevent future outbreaks.
Likely Candidates
People who live in hot climates are more likely to develop tinea versicolor than those who live in milder climates. According to the National Institutes of Health, male teenagers and young men are most commonly affected by this condition. People who sweat excessively also are more prone to develop tinea versicolor than people who do not.
Related Articles
References
- National Library of Medicine, Tinea Versicolor
- Harada K, Saito M, Sugita T, Tsuboi R. Malassezia species and their associated skin diseases. J Dermatol. 2015 Mar;42(3):250-7. doi:10.1111/1346-8138.12700
- Gupta AK, Foley KA. Antifungal treatment for pityriasis versicolor. J Fungi (Basel). 2015 Mar 12;1(1):13-29. doi:10.3390/jof1010013
- Hudson A, Sturgeon A, Peiris A. Tinea versicolor. JAMA. 2018 Oct 2;320(13):1396. doi:10.1001/jama.2018.12429
- Karray M, McKinney WP. Tinea (Pityriasis) Versicolor. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-. Updated April 1, 2019.
- Kaushik N, Pujalte GG, Reese ST. Superficial fungal infections. Prim Care. 2015 Dec;42(4):501-16. doi:10.1016/j.pop.2015.08.004
- Renati S, Cukras A, Bigby M. Pityriasis versicolor. BMJ. 2015 Apr 7;350:h1394. doi:10.1136/bmj.h1394
Writer Bio
Sophie Stillwell has been writing professionally since 1992. She is published in "The Gorham Times" newspaper, "Private Colleges & Universities" magazine, on eHow and in several other publications. She has experience working as a paralegal, antiques dealer and neurobehavioral coach. Her writing topics frequently include frugal living, pets and health. Stillwell holds a Bachelor of Arts in English from the University of Southern Maine.