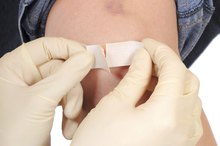
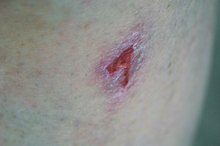
How to Treat Macerated Wounds
A macerated wound is an injury accompanied by soft, white, deteriorating skin around the site of the original injury. Maceration occurs when too much moisture is trapped between the wound and its bandage--sometimes the exudate (seepage of biological waste from the wound) escapes and gets trapped under the bandage, and sometimes the wound itself becomes overly moist. Maceration makes healing more difficult, so it should be carefully treated.
Remove any old bandages around the wound and inspect for signs of maceration. Decaying skin, putrefaction, or foul odors are signs of an infection that should be evaluated and treated by a medical professional. Lightly macerated tissue may be treated at home if the patient's condition does not decline.
How to Heal Broken Skin Fast
Learn More
Clean up any excess fluid from the wound site using sterile gauze pads. Check the wound itself for exudate and soak up as much as possible with the gauze.
Irrigate any wound that is packed with puss or other exudate. Use a clean syringe with sterile water to flush any residue from the wound, then soak up the water with sterile gauze. Just 2 oz. or less of water will suffice for most wounds.
How to Treat a Weeping Wound
Learn More
Treat the wound with an antiseptic/anesthetic cream or spray. Bacitracin or Neosporin are good choices 1. Just a drop or two of cream or a few pumps of the spray will be sufficient--the goal is to cover, not smother, the wound. Make sure the wound is moist but not wet.
Re-bandage the wound, using a bandage that is breathable.
Check the wound every four hours. Replace the bandage, soak up any new exudate, and check the progress of the maceration. If the wound's condition deteriorates, seek medical assistance.
Tips
If a wound becomes macerated even without exudate, then the problem is usually that the wound got wet and the bandage was not properly changed. There is no good reason, short of inadequate wound care, for a cut with little or no exudate to become macerated. Keep the wound moist without being wet, and change bandages after water immersion to avoid contamination.
Warnings
Maceration is a serious hindrance to wound healing and significantly improves the odds of infection. Watch the wound very carefully, and check the patient's temperature to identify signs of systemic infection. Macerated wounds are more likely to be damaged from secondary friction injuries, so if the wound is at a chafe point, take extra precautions to protect the wound, including the use of moleskin.
Related Articles
References
- Mccaughan D, Sheard L, Cullum N, Dumville J, Chetter I. Patients' perceptions and experiences of living with a surgical wound healing by secondary intention: A qualitative study. Int J Nurs Stud. 2018;77:29-38. doi:10.1016/j.ijnurstu.2017.09.015
- Krafts KP. Tissue repair: The hidden drama. Organogenesis. 2010;6(4):225-33. doi:10.4161/org.6.4.12555
- Chetter IC, Oswald AV, Fletcher M, Dumville JC, Cullum NA. A survey of patients with surgical wounds healing by secondary intention; an assessment of prevalence, aetiology, duration and management. J Tissue Viability. 2017;26(2):103-107. doi:10.1016/j.jtv.2016.12.004
- Singh PK, Saxena N, Poddar D, et al. Comparative Study Of Wound Healing In Primary Versus Delayed Primary Closure In Contaminated Abdominal Surgery. Hellenic J Surg. 2016;88:314–320. doi:10.1007/s13126-016-0340-8
- Surgical Patient Education Program: Prepare for the Best Recovery. American College of Surgeons. 2018.
- Rushbrook JL, White G, Kidger L, Marsh P, Taggart TF. The antibacterial effect of 2-octyl cyanoacrylate (Dermabond®) skin adhesive. J Infect Prev. 2014;15(6):236-239. doi:10.1177/1757177414551562
- Lazar HL, Mccann J, Fitzgerald CA, Cabral HJ. Adhesive strips versus subcuticular suture for mediansternotomy wound closure. J Card Surg. 2011;26(4):344-7. doi:10.1111/j.1540-8191.2011.01257.x
- 3M Wound Resource Center. http://solutions.3m.co.uk/wps/portal/3M/en_GB/skin-care/wound-resource-centre/
Tips
- If a wound becomes macerated even without exudate, then the problem is usually that the wound got wet and the bandage was not properly changed. There is no good reason, short of inadequate wound care, for a cut with little or no exudate to become macerated. Keep the wound moist without being wet, and change bandages after water immersion to avoid contamination.
Warnings
- Maceration is a serious hindrance to wound healing and significantly improves the odds of infection. Watch the wound very carefully, and check the patient's temperature to identify signs of systemic infection. Macerated wounds are more likely to be damaged from secondary friction injuries, so if the wound is at a chafe point, take extra precautions to protect the wound, including the use of moleskin.
Writer Bio
Jason Gillikin is a copy editor and writer who specializes in health care, finance and consumer technology. His various degrees in the liberal arts have helped him craft narratives within corporate white papers, novellas and even encyclopedias.