What does fact checked mean?
At Healthfully, we strive to deliver objective content that is accurate and up-to-date. Our team periodically reviews articles in order to ensure content quality. The sources cited below consist of evidence from peer-reviewed journals, prominent medical organizations, academic associations, and government data.
The information contained on this site is for informational purposes only, and should not be used as a substitute for the advice of a professional health care provider. Please check with the appropriate physician regarding health questions and concerns. Although we strive to deliver accurate and up-to-date information, no guarantee to that effect is made.
Melanoma & Weight Loss
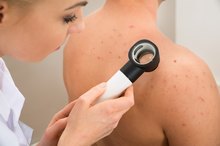
Melanoma is a type of cancer that forms in the cells that produces the melanin in your skin 1. Melanoma takes the lives of over 8,650 people every year -- although it is the most curable of all skin cancers, explains the American Cancer Society. If you have been recently diagnosed with melanoma, one of the first signs of the disease is weight loss. If you are experiencing weight loss and have a mole that has changed shape or color, see your doctor immediately.
Melanoma
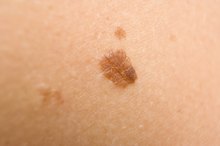
Melanoma occurs in people who have had excessive UV exposure but it can also stem from genetic and environmental factors, notes the Mayo Clinic. Melanoma generally starts off with a change in your existing mole or birth mark. Within the melanocytes, melanoma begins to take its shape 1. Following the basic ABCD and Es of melanoma, this tool can help you detect melanoma or other pre-cancerous skin lesions early on. Asymmetry. Think about what the mole would look like divided straight down the middle – if it would fold over to meet the same edges, it may be a sign of skin cancer. B stands for Border. Do you have a mole or skin spot that has a jagged edge? C is for color. Melanoma is known for turning an ugly color on your skin such as black, blue or gray – if the color of the mole changes colors or has other colors inside of it, it could be melanoma. D stands for diameter. A mole that is larger than the head of a pencil eraser should be examined. E is for elevation. A mole that rises above the skin’s surface needs to be looked at by a dermatologist.
- Melanoma occurs in people who have had excessive UV exposure but it can also stem from genetic and environmental factors, notes the Mayo Clinic.
- Melanoma is known for turning an ugly color on your skin such as black, blue or gray – if the color of the mole changes colors or has other colors inside of it, it could be melanoma.
Weight Loss
Differences between Malignant Melanoma and a Normal Mole
Learn More
Aside of recognizing that you have changes in your skin, you may also feel ill. One of the most common signs of skin cancer are feelings of generally malaise or like you have the flu. Headache, tiredness, feeling run down, loss of appetite and nausea are symptoms that your body is working to fight off the cancer and illness. Your loss of appetite can result in weight loss. If you have been recently diagnosed, weight loss could stem from the stress of the disease and the worry about your future health.
- Aside of recognizing that you have changes in your skin, you may also feel ill.
- If you have been recently diagnosed, weight loss could stem from the stress of the disease and the worry about your future health.
Stages
In advanced cases of melanoma, weight loss could be a sign that the disease has spread to surrounding lymph nodes or organs – this is called metastases. Metastases is common with melanoma because the cancer is very aggressive. Once the cancer spreads to other vital organs such as your liver, kidneys, lungs or brain, your body may respond through vomiting – making getting the right nutrition challenging.
- In advanced cases of melanoma, weight loss could be a sign that the disease has spread to surrounding lymph nodes or organs – this is called metastases.
Treatment
Early Signs of Skin Cancer and Penile Cancer
Learn More
Treating melanoma will be determined by your dermatologist and oncologist. Removal is almost always a priority as well as surgery in order to remove cancerous tumors or lymph nodes which the cancer cells that may have spread to. Another form of treatment is chemotherapy. Chemotherapy consists of a combination of nitrosoureas, methylating agents and taxanes, explains the University of Maryland Medical Center. Chemotherapy drugs can cause nausea, vomiting which can lead to extreme weight loss and malnutrition. Immunotherapy and radiation may also be considered, depending on the severity of your cancer.
- Treating melanoma will be determined by your dermatologist and oncologist.
- Chemotherapy consists of a combination of nitrosoureas, methylating agents and taxanes, explains the University of Maryland Medical Center.
Related Articles
References
- MedlinePlus: Metastatic Cancer to the Lung
- D'Orazio J, Jarrett S, Amaro-Ortiz A, Scott T. UV radiation and the skin. Int J Mol Sci. 2013;14(6):12222–12248. Published 2013 Jun 7. doi:10.3390/ijms140612222
- Riker AI, Zea N, Trinh T. The epidemiology, prevention, and detection of melanoma. Ochsner J. 2010;10(2):56–65. PMID: 21603359
- Bastian BC. The molecular pathology of melanoma: an integrated taxonomy of melanocytic neoplasia. Annu Rev Pathol. 2014;9:239–271. doi:10.1146/annurev-pathol-012513-104658
- McCourt C, Dolan O, Gormley G. Malignant melanoma: a pictorial review. Ulster Med J. 2014;83(2):103–110. PMID: 25075139
- Goodson AG, Grossman D. Strategies for early melanoma detection: Approaches to the patient with nevi. J Am Acad Dermatol. 2009;60(5):719–738. doi:10.1016/j.jaad.2008.10.065
- Ward WH. Clinical Presentation and Staging of Melanoma. Cutaneous Melanoma: Etiology and Therapy [Internet]. Published December 21, 2017.
- Liu Y, Sheikh MS. Melanoma: Molecular Pathogenesis and Therapeutic Management. Mol Cell Pharmacol. 2014;6(3):228. PMID: 25745537
- Corneli P, Zalaudek I, Magaton rizzi G, Di meo N. Improving the early diagnosis of early nodular melanoma: can we do better?. Expert Rev Anticancer Ther. 2018;18(10):1007-1012. doi:10.1080/14737140.2018.1507822
- Cohen LM. Lentigo maligna and lentigo maligna melanoma. J Am Acad Dermatol. 1995;33(6):923-36. doi:10.1016/0190-9622(95)90282-1
- Criscito MC, Stein JA. Improving the diagnosis and treatment of acral melanocytic lesions. Melanoma Manag. 2017;4(2):113–123. doi:10.2217/mmt-2016-0017
- Du F, Yang M, Fang J, Jing C. Primary hepatic malignant melanoma: a case report. Int J Clin Exp Pathol. 2015;8(2):2199–2201. Published 2015 Feb 1. PMID: 25973128
- Brahmer JR, Lacchetti C, Schneider BJ, et al. Management of Immune-Related Adverse Events in Patients Treated With Immune Checkpoint Inhibitor Therapy: American Society of Clinical Oncology Clinical Practice Guideline. J Clin Oncol. 2018;36(17):1714–1768. doi:10.1200/JCO.2017.77.6385
- Bertolotto C. Melanoma: from melanocyte to genetic alterations and clinical options. Scientifica (Cairo). 2013;2013:635203. doi:10.1155/2013/635203
- Institute for Quality and Efficiency in Health Care (IQWiG). What increases your risk of melanoma? InformedHealth.org [Internet]. Published November 29, 2018.
- Rangwala S, Tsai KY. Roles of the immune system in skin cancer. Br J Dermatol. 2011;165(5):953–965. doi:10.1111/j.1365-2133.2011.10507.x
- Gupta AK, Bharadwaj M, Mehrotra R. Skin Cancer Concerns in People of Color: Risk Factors and Prevention. Asian Pac J Cancer Prev. 2016;17(12):5257–5264. Published 2016 Dec 1. doi:10.22034/APJCP.2016.17.12.5257
- Wu S, Cho E, Li WQ, Weinstock MA, Han J, Qureshi AA. History of Severe Sunburn and Risk of Skin Cancer Among Women and Men in 2 Prospective Cohort Studies. Am J Epidemiol. 2016;183(9):824–833. doi:10.1093/aje/kwv282
- Kaliyadan F. The scope of the dermoscope. Indian Dermatol Online J. 2016;7(5):359–363. doi:10.4103/2229-5178.190496
- Abbasi NR, Shaw HM, Rigel DS, et al. Early diagnosis of cutaneous melanoma: revisiting the ABCD criteria. JAMA. 2004;292(22):2771-6. doi:10.1001/jama.292.22.2771
- Shenenberger DW. Cutaneous malignant melanoma: a primary care perspective. Am Fam Physician. 2012;85(2):161-8. PMID: 22335216
- Bennett JP, Hall P. Moles and melanoma: a history. Ann R Coll Surg Engl. 1994;76(6):373–380. PMID: 7702317
- Gaudy-marqueste C, Wazaefi Y, Bruneu Y, et al. Ugly Duckling Sign as a Major Factor of Efficiency in Melanoma Detection. JAMA Dermatol. 2017;153(4):279-284. doi:10.1001/jamadermatol.2016.5500
- Mohr P, Eggermont AM, Hauschild A, Buzaid A. Staging of cutaneous melanoma. Ann Oncol. 2009;20 Suppl 6(Suppl 6):vi14–vi21. doi:10.1093/annonc/mdp256
- PDQ Adult Treatment Editorial Board. Melanoma Treatment (PDQ®): Patient Version. 2019 Nov 8. In: PDQ Cancer Information Summaries [Internet]. Bethesda (MD): National Cancer Institute (US); 2002-.
- Erdei E, Torres SM. A new understanding in the epidemiology of melanoma. Expert Rev Anticancer Ther. 2010;10(11):1811–1823. doi:10.1586/era.10.170
- Wernick BD, Goel N, Zih FS, Farma JM. A surgical perspective report on melanoma management. Melanoma Manag. 2017;4(2):105–112. doi:10.2217/mmt-2016-0031
- Bagaria SP, Faries MB, Morton DL. Sentinel node biopsy in melanoma: technical considerations of the procedure as performed at the John Wayne Cancer Institute. J Surg Oncol. 2010;101(8):669–676. doi:10.1002/jso.21581
- Sadozai H, Gruber T, Hunger RE, Schenk M. Recent Successes and Future Directions in Immunotherapy of Cutaneous Melanoma. Front Immunol. 2017;8:1617. Published 2017 Dec 8. doi:10.3389/fimmu.2017.01617
- Mattia G, Puglisi R, Ascione B, Malorni W, Carè A, Matarrese P. Cell death-based treatments of melanoma:conventional treatments and new therapeutic strategies. Cell Death Dis. 2018;9(2):112. Published 2018 Jan 25. doi:10.1038/s41419-017-0059-7
- Testori A, Rutkowski P, Marsden J, et al. Surgery and radiotherapy in the treatment of cutaneous melanoma. Ann Oncol. 2009;20 Suppl 6(Suppl 6):vi22–vi29. doi:10.1093/annonc/mdp257
- Glanz K, Buller DB, Saraiya M. Reducing ultraviolet radiation exposure among outdoor workers: state of the evidence and recommendations. Environ Health. 2007;6:22. Published 2007 Aug 8. doi:10.1186/1476-069X-6-22
- Autier P. Do high factor sunscreens offer protection from melanoma?. West J Med. 2000;173(1):58. doi:10.1136/ewjm.173.1.58
- Le Clair MZ, Cockburn MG. Tanning bed use and melanoma: Establishing risk and improving prevention interventions. Prev Med Rep. 2016;3:139–144. Published 2016 Jan 14. doi:10.1016/j.pmedr.2015.11.016
- Weinstock MA, Risica PM, Martin RA, et al. Melanoma early detection with thorough skin self-examination: the "Check It Out" randomized trial. Am J Prev Med. 2007;32(6):517–524. doi:10.1016/j.amepre.2007.02.024
- InformedHealth.org [Internet]. Cologne, Germany: Institute for Quality and Efficiency in Health Care (IQWiG); 2006-. Detecting melanoma. 2015 Sep 10 [Updated 2018 Nov 29].
- Walter FM, Humphrys E, Tso S, Johnson M, Cohn S. Patient understanding of moles and skin cancer, and factors influencing presentation in primary care: a qualitative study. BMC Fam Pract. 2010;11:62. Published 2010 Aug 31. doi:10.1186/1471-2296-11-62
- Bode AM, Dong Z. Cancer prevention research - then and now. Nat Rev Cancer. 2009;9(7):508–516. doi:10.1038/nrc2646
- How to Do a Skin Self-Exam. American Cancer Society. Published July 23, 2019.
Writer Bio
Julie Boehlke is a seasoned copywriter and content creator based in the Great Lakes state. She is a member of the Society of Professional Journalists. Boehlke has more than 10 years of professional writing experience on topics such as health and wellness, green living, gardening, genealogy, finances, relationships, world travel, golf, outdoors and interior decorating. She has also worked in geriatrics and hospice care.