Leg, Ball & Socket Pain
Your legs and the connecting ball and socket joints rely on one another to perform singular tasks. Often when one hurts, it affects the other. There are a number of reasons why your leg and the connecting ball and socket joint are in pain. The treatments also vary, depending on the cause.
If you are experiencing serious medical symptoms, seek emergency treatment immediately.
Identification
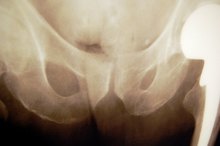
The ball and socket joint associated with your leg is your hip joint. It is one of the most stable joints in your body. The ball is the femoral head and is at the top of the thighbone. The socket is part of your pelvis. In order for the ball of the hip joint to move smoothly in the socket, the surfaces of each are coated with articular cartilage. The edge of the socket consists of fibrous tissue and cartilage, which helps deepen the socket and improve stability.
- The ball and socket joint associated with your leg is your hip joint.
- In order for the ball of the hip joint to move smoothly in the socket, the surfaces of each are coated with articular cartilage.
Significance
Causes of Nerve Pain in the Hip & Leg
Learn More
Your legs, thanks to your hips, support your body, giving it stability. When any part of the hip is damaged or injured, it can be felt all the way down the leg to the ankle. An injury of the hip can also affect how you walk. The longest muscle in the body, the elongated sartorious muscle, which is located in the thigh, connects the knee to the hip joint. Two other muscles located in the thigh, the rectus femoris and the semi-tendonous fusiform, can also affect the hip joint.
- Your legs, thanks to your hips, support your body, giving it stability.
- The longest muscle in the body, the elongated sartorious muscle, which is located in the thigh, connects the knee to the hip joint.
Causes
Leg and hip pain can be caused by an organic disease, such as a misalignment or fracture of the spine 4. The pain can also be from cancerous cells that attack the lower spine or the leg and hip muscles 4. If an insufficient amount of blood flows to the hip, commonly seen in those with sickle cell anemia, aseptic necrosis may develop. Degenerative diseases can also cause pain in the leg and hip joint 4. Osteoporosis causes a decrease in bone density and the muscle and nerve endings can deteriorate, resulting in pain and swelling.
Treatment
Causes of Fever & Pain in the Leg
Learn More
If you have a misalignment of your spine, a visit to the chiropractor may be in order. A fractured spine requires pain management and stabilization. Braces, orthotics and sometimes surgery may be needed. Cancer is often treated with chemotherapy or radiation. Aseptic necrosis is treated by treating the underlying condition. However, surgery is often needed. Osteoporosis treatment typically includes nutrition, exercise, supplements or prescribed medication.
- If you have a misalignment of your spine, a visit to the chiropractor may be in order.
- A fractured spine requires pain management and stabilization.
Related Articles
References
Writer Bio
Nicole Adams is an accomplished writer, publishing in print and online. She has submitted hundreds of articles for websites, including CBS Local and Education.com. Adams earned a Bachelor of Science in psychology with concentrated studies in health and nutrition, and animal behavior and nutrition. She loves to cook and volunteers in animal rescue.