Pain From a Torn LCL Ligament When Walking
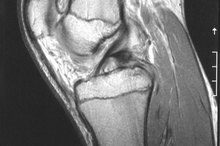
Pain from a damaged LCL, or lateral collateral ligament, occurs on the outside of your knee. The LCL runs from the top part of your fibula, which is the bone on the outside of your lower leg, to the exterior lower thighbone. The ligament is designed to keep your knee stable. There are a number of reasons you might experience pain in your knee while walking, although it usually happens after an injury, according to MedlinePlus.
Symptoms
One sign that you have a torn LCL is that you'll feel unsteady on your feet and feel like you might fall while you're walking. Conversely, your knee might lock while you're walking, making it difficult to bend your knee. You may experience tenderness or swelling, which worsens the longer you move. Pain can be severe or just mildly irritating. The swelling often traps the nerves in your legs and you may feel your foot lose feeling as you walk.
Causes
Pain in the Knee & Occasional Popping When Walking
Learn More
It's usually a direct blow to the outside of your knee that causes a tear in the LCL. LCL tears commonly occur after car and bicycle accidents when you bump your knee on a hard surface with sufficient force to tear the ligament. Athletes who participate in sports that require numerous starts and stops such as basketball, soccer and skiing commonly tear their LCL ligaments during play. Football and hockey players also receive ligament tears when pounded on the knee. Repeated stress also can lead to eventual tears.
Treatment
Mild LDL tears usually heal with rest, according to Cedars-Sinai Medical Center, although they may take longer to repair than other ligaments -- up to six months. You may have to wear a brace to continue walking as well as use over-the-counter anti-inflammatory pain relievers such as ibuprofen. A special cast allows you to keep walking because it has a hole in the knee portion of the cast, but it restricts your knee from moving side to side. Surgery may be required if the ligament was torn from either of the bones to which it is attached.
Prevention
Exercises for a Torn Quad
Learn More
The best way to prevent a torn LCL is to use proper techniques when you're walking or playing sports and not to fall or get hit. By strengthening your thigh and leg muscles, you'll provide additional support for your knee ligaments and be able to prevent accidents. Additionally, your muscles should take the brunt of your movements, allowing your ligaments to serve in the capacity for which they were intended, to keep your knees in place.
Related Articles
References
Resources
Writer Bio
Linda Ray is an award-winning journalist with more than 20 years reporting experience. She's covered business for newspapers and magazines, including the "Greenville News," "Success Magazine" and "American City Business Journals." Ray holds a journalism degree and teaches writing, career development and an FDIC course called "Money Smart."