How Long Until a Chipped Bone on the Knee From Playing Football Heals?
Football is a high-impact sport that can take its toll on your body. Sprinting, sudden starts and stops and direct collisions can lead to injuries of the knees.
If you are experiencing serious medical symptoms, seek emergency treatment immediately.
Chipped bones in your knee often result from a previous injury that causes bone or cartilage pieces to chip off. This condition is known as osteochondritis dissecans, and it should be treated by a physician to promote proper healing. A chipped bone in the knee can take weeks or months to heal, according to Cedars Sinai Orthopaedic Center.
Osteochondritis Dissescans
Osteochondritis dissecans occurs most often in young men, especially those who have sustained prior joint injuries, according to the Mayo Clinic. When pieces of bone or cartilage chip from the knee, the fragment may become jammed between the moving portions of your knee joint. This can lead to pain, especially during sports and star climbing [1](# 'inline-reference::"The Sports Medicine Patient Advisor"; Pierre Rouzier, et al.
; 2004').
If you have osteochondritis dissecans, you also might notice joint locking or popping as you move. Your knee joint may feel weak, have a limited range of motion or appear swollen and tender. Some individuals with this condition may never experience symptoms.
- Osteochondritis dissecans occurs most often in young men, especially those who have sustained prior joint injuries, according to the Mayo Clinic.
- If you have osteochondritis dissecans, you also might notice joint locking or popping as you move.
Diagnosis
Pain in the Knee & Occasional Popping When Walking
Learn More
If you experience persistent knee pain, see a physician and discontinue football until he says otherwise. the doctor will perform a physical examination and review your medical history [1](# 'inline-reference::"The Sports Medicine Patient Advisor"; Pierre Rouzier, et al.
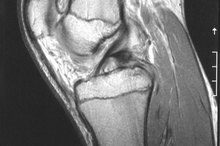
; 2004'). Your doctor might take X-rays of your knee to rule out other conditions. Further imaging studies, such as CT scans or MRIs, may provide a more detailed view of your knee joint to help your doctor determine where chipped bone is present and what he needs to do to treat your condition.
- If you experience persistent knee pain, see a physician and discontinue football until he says otherwise.
- Further imaging studies, such as CT scans or MRIs, may provide a more detailed view of your knee joint to help your doctor determine where chipped bone is present and what he needs to do to treat your condition.
Treatment
The goal of treatment of osteochondritis dissecans is to restore normal function of your knee and to reduce pain. Docs generally try conservative measures first to relieve your pain. Your doctor may recommend avoiding high-impact physical activities such as football and participation in low-impact exercise, such as swimming or using an elliptical machine. You may also be required to use crutches to allow your knee to rest.
Physical therapy might help increase strength and range of motion in your knee joint. If conservative treatment fails, surgery might be necessary to remove bone chips.
- The goal of treatment of osteochondritis dissecans is to restore normal function of your knee and to reduce pain.
- Physical therapy might help increase strength and range of motion in your knee joint.
Recovery Time
How Long Does it Take to Rehab From Meniscus Surgery?
Learn More
The recovery time for treatment for osteochondritis dissecans largely depends on the type of treatment used. Cedars Sinai Orthopaedic Center indicates that competitive sports and physical activities should be avoided for six to eight weeks. During this time, a knee brace or crutches may be used. If after three to six months of conservative treatment, your doctor may recommend surgery. Surgery may be performed by completely opening the knee or with arthroscopic surgery.
The recovery time for arthroscopic surgery tends to be shorter than having opened knee surgery. Only your doctor can provide you with an exact recovery time from surgery based on the severity of your condition and how well your body handles surgery and rehabilitation.
- The recovery time for treatment for osteochondritis dissecans largely depends on the type of treatment used.
- The recovery time for arthroscopic surgery tends to be shorter than having opened knee surgery.
Returning to Football
Your return to football largely depends on your pain level, as well as the type of treatment you received. Ultimately, you and your doctor will make the decision [1](# 'inline-reference::"The Sports Medicine Patient Advisor"; Pierre Rouzier, et al.
; 2004'). You should not return to football until you have regained strength in your knee and are able to run and spring without limping. Your knee should not be swollen or tender. You should be able to jump without pain, cut back and forth on the football field and run figure-eights without experiencing pain.
- Your return to football largely depends on your pain level, as well as the type of treatment you received.
- You should not return to football until you have regained strength in your knee and are able to run and spring without limping.
Related Articles
References
- "The Sports Medicine Patient Advisor"; Pierre Rouzier, et al.; 2004
- Lespasio MJ, Piuzzi NS, Husni ME, Muschler GF, Guarino A, Mont MA. Knee Osteoarthritis: A Primer. Perm J. 2017;21:16-183. doi:10.7812/TPP/16-183
- Kiapour AM, Murray MM. Basic science of anterior cruciate ligament injury and repair. Bone Joint Res. 2014;3(2):20-31. doi:10.1302/2046-3758.32.2000241
- Doral MN, Bilge O, Huri G, Turhan E, Verdonk R. Modern treatment of meniscal tears. EFORT Open Rev. 2018;3(5):260-268. doi:10.1302/2058-5241.3.170067
- Reinking MF. CURRENT CONCEPTS IN THE TREATMENT OF PATELLAR TENDINOPATHY. Int J Sports Phys Ther. 2016;11(6):854-866.
- Petersen W, Rembitzki I, Liebau C. Patellofemoral pain in athletes. Open Access J Sports Med. 2017;8:143-154. doi:10.2147/OAJSM.S133406
- Frush TJ, Noyes FR. Baker's Cyst: Diagnostic and Surgical Considerations. Sports Health. 2015;7(4):359-65. doi:10.1177/1941738113520130
- Huang YC, Yeh WL. Endoscopic treatment of prepatellar bursitis. Int Orthop. 2011;35(3):355-8. doi:10.1007/s00264-010-1033-5
- Beals C, Flanigan D. A Review of Treatments for Iliotibial Band Syndrome in the Athletic Population. J Sports Med (Hindawi Publ Corp). 2013;2013:367169. doi:10.1155/2013/367169
- Tsai CH, Hsu CJ, Hung CH, Hsu HC. Primary traumatic patellar dislocation. J Orthop Surg Res. 2012;7:21. doi:10.1186/1749-799X-7-21
- Ragab G, Elshahaly M, Bardin T. Gout: An old disease in new perspective - A review. J Adv Res. 2017;8(5):495-511. doi:10.1016/j.jare.2017.04.008
- Lee PYF, Nixion A, Chandratreya A, Murray JM. Synovial Plica Syndrome of the Knee: A Commonly Overlooked Cause of Anterior Knee Pain. Surg J (N Y). 2017;3(1):e9-e16. doi:10.1055/s-0037-1598047
- Vaishya R, Azizi AT, Agarwal AK, Vijay V. Apophysitis of the Tibial Tuberosity (Osgood-Schlatter Disease): A Review. Cureus. 2016;8(9):e780. doi:10.7759/cureus.780
- Zanon G, Di vico G, Marullo M. Osteochondritis dissecans of the knee. Joints. 2014;2(1):29-36.
- Hindle P, Davidson E, Biant LC. Septic arthritis of the knee: the use and effect of antibiotics prior to diagnostic aspiration. Ann R Coll Surg Engl. 2012;94(5):351-5. doi:10.1308/003588412X13171221591015
- Gwinner C, Märdian S, Schwabe P, Schaser KD, Krapohl BD, Jung TM. Current concepts review: Fractures of the patella. GMS Interdiscip Plast Reconstr Surg DGPW. 2016;5:Doc01. doi:10.3205/iprs000080
- Voskuil R, Evenski AJ, Montgomery C, Emory CL. Malignant Bone Tumors of the Knee: How to Identify and Treat. J Knee Surg. 2019;32(4):305-314. doi:10.1055/s-0038-1675828
- Gupte C, St mart JP. The acute swollen knee: diagnosis and management. J R Soc Med. 2013;106(7):259-68. doi:10.1177/0141076813482831
- American Academy of Orthopedic Surgeons. Unstable Kneecap.
- Bhatia D, Bejarano T, Novo M. Current interventions in the management of knee osteoarthritis. Journal of Pharmacy & Bioallied Sciences 2013 Jan-Mar;5(1):30-38. doi:%2010.4103/0975-7406.106561
- Bronstein RD, Schaffer JC. Physical Examination of the Knee: Meniscus, Cartilage, and Patellofemoral Conditions. J Am Acad Orthop Surg. 2017 May;25(5):365-374.
- Browne K, Kurtz CA. How to perform a comprehensive examination of the knee. JAAPA. 2009 Jun;22(6):20-25.
- Hergenroeder AC, Harvey BS. (2017). Osteochondritis dissecans (OCD): Clinical manifestations and diagnosis. Bachur RG, ed. UpToDate. Waltham, MA: UpToDate Inc.
Writer Bio
Michelle Zehr started writing professionally in 2009. She has written on health, fitness, fashion, interior design, home decorating,sports and finance for several websites. Zehr possesses a Bachelor of Arts in communication from the University of Pittsburgh, a Master of Arts in professional writing from Chatham University and a graduate certificate in health promotion from California University of Pennsylvania.