How to Check for a Broken Tail Bone
The coccyx, more commonly called the tailbone, is the small structure at the bottom of your spine composed of three to five fragments 2. If a tailbone becomes injured, there is moderate to severe discomfort in the general area. The majority of tailbone injuries occur in females due to their wider pelvises. Even with proper treatment, broken tailbones take some time to heal.
If you are experiencing serious medical symptoms, seek emergency treatment immediately.
Feel for tenderness and note any severe pain in the immediate tailbone area. Direct pressure to the tailbone will cause immediate pain to anyone with a broken coccyx 2. Touching or rubbing the spot or even sitting down may cause pain. Even sitting on a pillow for long periods may cause discomfort depending on the severity of the injury.
How to Treat a Deep Bone Bruise of the Knee
Learn More
Inspect the skin for any bruising. While bruising does not necessarily mean the tailbone is broken, it is a common sign there is an injury 2. If a bruise is not visible, feel for a knot or swollen hump. This may be the bone protruding outward to the skin.
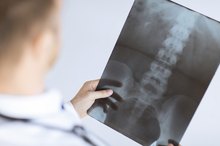
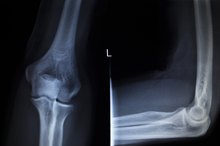
Visit the doctor for a vertebral column test. The test can tell if any part of the spinal column is injured. The doctor may need to perform a rectal examination to feel the coccyx and determine if it is dislocated. The doctor may also take an X-ray to locate a fracture or dislocation.
How to Treat Pelvic Hairline Fracture
Learn More
Treat the injury at home if you think the tailbone is broken and you cannot visit a doctor immediately 2. Apply ice to the injury for about 20 minutes, four times per day, until you can seek medical treatment. Avoid applying direct weight to the tailbone by leaning forward when sitting down. Refrain from activities that require the use of your lower back such as weight lifting or sexual intercourse.
Warnings
Always consult a doctor for a proper diagnosis.
Related Articles
References
- EMedicine Health: Tailbone (Coccyx) Injury
- WebMD: Tailbone (Coccyx) Injury
- Blocker O, Hill S, Woodacre T. Persistent coccydynia--the importance of a differential diagnosis. BMJ Case Rep. 2011;2011:bcr0620114408. doi:10.1136/bcr.06.2011.4408
- Foye PM, Abdelshahed DM, Kamrava E, Enriquez R, D'onofrio GJ. Tailbone Pain from Coccyx Injuries on Water Slides: A Case Series. J Emerg Med. 2018;55(2):e33-e35. doi:10.1016/j.jemermed.2018.04.033
- Young JD, Gelbs JC, Zhu DS, Gallacher SE, Sutton KM, Blaine TA. Orthopaedic Injuries in Equestrian Sports: A Current Concepts Review. Orthop J Sports Med. 2015;3(9):2325967115603924. doi:10.1177/2325967115603924
- Márquez-carrasco ÁM, García-garcía E, Aragúndez-marcos MP. Coccyx pain in women after childbirth. Enferm Clin. 2019;29(4):245-247. doi:10.1016/j.enfcli.2019.01.005
- Gonnade N, Mehta N, Khera PS, Kumar D, Rajagopal R, Sharma PK. Ganglion impar block in patients with chronic coccydynia. Indian J Radiol Imaging. 2017;27(3):324–328. doi:10.4103/ijri.IJRI_294_16
- Faubion SS, Shuster LT, Bharucha AE. Recognition and management of nonrelaxing pelvic floor dysfunction. Mayo Clin Proc. 2012;87(2):187–193. doi:10.1016/j.mayocp.2011.09.004
- Uglialoro AD, Beebe KS, Hameed M, Benevenia J. A rare case of intraosseous benign notochordal cell tumor of the coccyx. Orthopedics. 2009;32(6):445. doi:10.3928/01477447-20090511-22
- Nunes LF, Castro Neto AK, Vasconcelos RA, et al. Carcinomatous degeneration of pilonidal cyst with sacrum destruction and invasion of the rectum. An Bras Dermatol. 2013;88(6 Suppl 1):59–62. doi:10.1590/abd1806-4841.20132140
- Dudareva M, Ferguson J, Riley N, Stubbs D, Atkins B, McNally M. Osteomyelitis of the Pelvic Bones: A Multidisciplinary Approach to Treatment. J Bone Jt Infect. 2017;2(4):184–193. doi:10.7150/jbji.21692
- Saleem S, Aslam HM, Rehmani MA, Raees A, Alvi AA, Ashraf J. Lumbar disc degenerative disease: disc degeneration symptoms and magnetic resonance image findings. Asian Spine J. 2013;7(4):322–334. doi:10.4184/asj.2013.7.4.322
- Jeyarajah S, Purkayastha S. Proctalgia fugax. CMAJ. 2013;185(5):417. doi:10.1503/cmaj.101613
- Lirette LS, Chaiban G, Tolba R, Eissa H. Coccydynia: an overview of the anatomy, etiology, and treatment of coccyx pain. Ochsner J. 2014;14(1):84–87.
- Malanga GA, Yan N, Stark J. Mechanisms and efficacy of heat and cold therapies for musculoskeletal injury. Postgrad Med. 2015;127(1):57-65. doi:10.1080/00325481.2015.992719
- Scott KM, Fisher LW, Bernstein IH, Bradley MH. The Treatment of Chronic Coccydynia and Postcoccygectomy Pain With Pelvic Floor Physical Therapy. PM R. 2017;9(4):367-376. doi:10.1016/j.pmrj.2016.08.007
- Antoniadis A, Ulrich NH, Senyurt H. Coccygectomy as a surgical option in the treatment of chronic traumatic coccygodynia: a single-center experience and literature review. Asian Spine J. 2014;8(6):705–710. doi:10.4184/asj.2014.8.6.705
- Foye PM. Coccydynia: Tailbone Pain. Phys Med Rehabil Clin N Am. 2017 Aug;28(3):539-49.
- Lirette LS, Chaiban G, Tolba R, Eissa H. Coccydynia: An Overview of the Anatomy, Etiology, and Treatment of Coccyx Pain. Ochsner J. 2014 Spring;14(1):84-87.
- Nathan ST, Fisher BE, Roberts CS. Coccydynia: a review of pathoanatomy, aetiology, treatment and outcome. J Bone Joint Surg Br. 2010 Dec;92(12):1622-7.
Warnings
- Always consult a doctor for a proper diagnosis.
Writer Bio
Corey Morris has been writing since 2009. He has been a reporter for his campus newspaper, "The Rotunda" and is the publication's news editor. His work focuses on topics in news, politics and community events. He is pursuing a Bachelor of Science in political science and mass media from Longwood University in Farmville, Va.