What does fact checked mean?
At Healthfully, we strive to deliver objective content that is accurate and up-to-date. Our team periodically reviews articles in order to ensure content quality. The sources cited below consist of evidence from peer-reviewed journals, prominent medical organizations, academic associations, and government data.
The information contained on this site is for informational purposes only, and should not be used as a substitute for the advice of a professional health care provider. Please check with the appropriate physician regarding health questions and concerns. Although we strive to deliver accurate and up-to-date information, no guarantee to that effect is made.
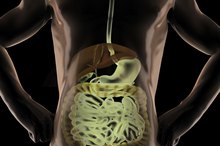
A gastric ulcer is painful, but it's usually not life-threatening. An ulcer in the liver--more correctly called a liver abscess--is a more serious condition that requires medical intervention to prevent possible sepsis and death. Those who are vulnerable to liver ulcers need to be aware of the symptoms so they can begin treatment as soon as possible.
If you are experiencing serious medical symptoms, seek emergency treatment immediately.
Types
The condition referred to as a liver ulcer may be one of two things 2. On occasion, a peptic ulcer--an ulcer in the stomach, duodenum or esophagus--may penetrate into the liver. This is a rare condition. More commonly, a liver ulcer is actually a liver abscess or an area of the liver that becomes infected and filled with pus.
- The condition referred to as a liver ulcer may be one of two things 2.
- More commonly, a liver ulcer is actually a liver abscess or an area of the liver that becomes infected and filled with pus.
Causes
Causes of Spots on the Liver
Learn More
A liver abscess is caused by infection in the abdomen, blood or biliary tract. Sometimes such an infection can be caused by an endoscopy of the biliary system or by any trauma to the liver. It can also be a result of appendicitis, diverticulitis or a perforated bowel. Usually, more than one type of bacteria is found in a liver infection. Bacteroides, enterococcus, escherichia colie, klebsiella staphylococcus or streptococcus are the most common kinds of bacteria that cause this type of infection. A peptic ulcer is also generally caused by bacteria.
- A liver abscess is caused by infection in the abdomen, blood or biliary tract.
- Bacteroides, enterococcus, escherichia colie, klebsiella staphylococcus or streptococcus are the most common kinds of bacteria that cause this type of infection.
Symptoms
For a peptic ulcer that has extended into the liver, gastrointestinal bleeding is the most common symptom. With a liver abscess, patients may experience pain in the upper abdomen, loss of appetite, nausea, vomiting and unexpected weight loss. Other signs include dark urine, chalk-colored stool and jaundice, or yellow-tinted skin. Patients may also have weakness and fever or chills.
- For a peptic ulcer that has extended into the liver, gastrointestinal bleeding is the most common symptom.
- With a liver abscess, patients may experience pain in the upper abdomen, loss of appetite, nausea, vomiting and unexpected weight loss.
Diagnosis
What Are the Treatments for a Liver Cyst?
Learn More
Doctors can use endoscopy to diagnose a peptic ulcer that extends into the liver 2. For a liver abscess, doctors use a liver biopsy, abdominal ultrasound or abdominal computed axial tomography (CT) scan to diagnose. A white blood cell count, blood culture for bacteria or liver function test are other ways to diagnose this condition.
Treatment
In most cases, patients require surgery to drain the pus from the liver, followed by an intense course of antibiotics for four to six weeks. In a few cases, antibiotic treatment alone may work. Antibiotics and antacids are used to treat peptic ulcers. Left untreated, liver abscess may be fatal, so no patient should ignore his symptoms and hope the pain will go away on its own.
- In most cases, patients require surgery to drain the pus from the liver, followed by an intense course of antibiotics for four to six weeks.
- Left untreated, liver abscess may be fatal, so no patient should ignore his symptoms and hope the pain will go away on its own.
Related Articles
References
- MedLine Plus: Pyogenic Liver Abscess
- World Journal of Gastroentology: Gastric Ulcer Penetrating to Liver Diagnosed by Endoscopic Biopsy
- Ramakrishnan K, Salinas RC. Peptic ulcer disease. Am Fam Physician. 2007;76(7):1005-12.
- Azhari H, Underwood F, King J, et al. A36 THE GLOBAL INCIDENCE OF PEPTIC ULCER DISEASE AND ITS COMPLICATIONS AT THE TURN OF THE 21ST CENTURY: A SYSTEMATIC REVIEW. Journal of the Canadian Association of Gastroenterology. 2018;1(2):61-62. doi:10.1093/jcag/gwy009.036
- Malik TF, Singh K. Peptic Ulcer Disease. StatPearls Publishing. Updated December 4, 2018.
- Nelms DW, Pelaez CA. The Acute Upper Gastrointestinal Bleed. Surg Clin North Am. 2018;98(5):1047-1057. doi:10.1016/j.suc.2018.05.004
- Saljoughian M. Gastrointestinal Bleeding: An Alarming Sign. US Pharm. 2009;34(12):HS12-HS16.
- Testerman TL, Morris J. Beyond the stomach: an updated view of Helicobacter pylori pathogenesis, diagnosis, and treatment. World J Gastroenterol. 2014;20(36):12781-808. doi:10.3748/wjg.v20.i36.12781
- American College of Gastroenterology. Peptic Ulcer Disease.
- Vomero ND, Colpo E. Nutritional care in peptic ulcer. Arq Bras Cir Dig. 2014;27(4):298-302. doi:10.1590/S0102-67202014000400017
- Lau JY, Sung J, Hill C, et al. Systematic Review of the Epidemiology of Complicated Peptic Ulcer Disease: Incidence, Recurrence, Risk Factors and Mortality. Digestion, 2011; 84:102. doi:10.1159/000323958
- Li LF, Chan RL, Lu L, et al. Cigarette Smoking and Gastrointestinal Diseases: the Causal Relationship and Underlying Molecular Mechanisms (Review). Int J Mol Med,2014; 34:372. doi:10.3892/ijmm.2014.1786
- Malfertheiner P, Megraud F, O'Morain CA, et al. Management of Helicobacter Pylori Infection--the Maastricht IV/ Florence Consensus Report. Gut, 2012; 61:646. doi:10.1136/gutjnl-2012-302084
Writer Bio
Anne Madison has been a freelance writer since 2005. Her fiction has appeared in several magazines, including "Let's Worship" and "Drama Ministry." She has published numerous articles on eHow and other websites.