What does fact checked mean?
At Healthfully, we strive to deliver objective content that is accurate and up-to-date. Our team periodically reviews articles in order to ensure content quality. The sources cited below consist of evidence from peer-reviewed journals, prominent medical organizations, academic associations, and government data.
- MedlinePlus: Total Colectomy or Proctocolectomy: Discharge
- Cleveland Clinic: Total Abdominal Colectomy: Basic Surgical Steps
The information contained on this site is for informational purposes only, and should not be used as a substitute for the advice of a professional health care provider. Please check with the appropriate physician regarding health questions and concerns. Although we strive to deliver accurate and up-to-date information, no guarantee to that effect is made.
Diet After Total Abdominal Colectomy
Inflammatory bowel disease, cancer of the colon or other conditions that damage your large intestine may require a total abdominal colectomy 2. After the procedure, your doctor will order a diet that gives your intestinal tract time to heal. As you progress through your recovery, your diet will gradually include more substantial foods until you’re back to your regular eating plan. In the months following your procedure, eat a nutritious, balanced diet rich in nutrients that help your body heal and fight infection.
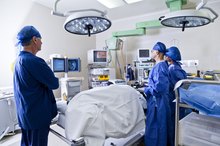
Procedure
During a total abdominal colectomy, sometimes known as an ileorectal anastomosis, the surgeon removes your entire large intestine from the final segment of the small intestine, or ileum, to the rectum 2. Then the surgeon creates a connection, or anastomosis, between the end of your ileum and your rectum or anus. Alternatively, your surgeon may create an internal pouch for stool collection, using a portion of your small intestine. Crohn’s disease, ulcerative colitis, colon cancer and other conditions that have damaged your large intestine without affecting your rectum may warrant a total abdominal colectomy 2. Your doctor may also recommend this procedure for severe constipation caused by inadequate muscle or nerve function, a condition called colonic inertia.
Post-Surgical Nutrition
Splenectomy & Diet
Learn More
Immediately after surgery, you will receive nutrients and fluids intravenously, or through your veins. After one to two days, your doctor may advance you to a clear liquid diet, according to the University of Maryland Medical Center, or UMMC. A clear liquid diet consists of water, juices without pulp, broth, electrolyte replacement drinks, gelatin and ice pops. This diet allows your intestinal tract to rest while the newly created connection between your ileum and rectum or anus heals.
- Immediately after surgery, you will receive nutrients and fluids intravenously, or through your veins.
- After one to two days, your doctor may advance you to a clear liquid diet, according to the University of Maryland Medical Center, or UMMC.
Recovery
When you’re able to tolerate liquids, your doctor will gradually advance you to a low-residue diet consisting of soft foods that have little or no indigestible fiber. Low-residue foods leave very little undigested material for your intestine to process, according to the University of Pittsburgh Medical Center. The diet also restricts milk products and foods or beverages that contain caffeine. As you’re recovering, eating white bread, crackers, skinless potatoes, white rice, yogurt, tender ground meat and canned fruits and vegetables without skins and other low-fiber foods will provide nutrients without jeopardizing the results of your surgery. MedlinePlus advises that you eat five to eight meals each day, spaced evenly throughout the day, in this phase of your recovery. Your surgeon or doctor will determine how long you should follow a low-residue diet. A low-residue diet and pain medication may cause constipation. Consult your surgeon for recommendations about adequate fluid intake and fiber supplements to restore regular bowel movements.
- When you’re able to tolerate liquids, your doctor will gradually advance you to a low-residue diet consisting of soft foods that have little or no indigestible fiber.
- Your surgeon or doctor will determine how long you should follow a low-residue diet.
Healing
Diet After a Frenectomy
Learn More
After you’ve recovered from surgery, you should be able to perform most of your usual activities, the UMMC notes. You may have an increased number of bowel movements -- four to six per day -- because of alterations in your digestive tract.
When you’re ready to progress to a regular diet, include foods that support your immune system and promote healthy wound healing. Protein from lean meat, fish and poultry, soy products, eggs and dairy foods will give your body the materials it needs to rebuild and repair tissues. Vitamins A and C play roles in tissue regeneration and boost your immune system. Citrus fruits, tomatoes, potatoes, and dark green vegetables are rich in vitamin C. Milk, eggs, liver and orange, red and yellow vegetables contain vitamin A or its precursor, beta-carotene. Your diet should also include foods rich in zinc, an essential mineral involved in wound repair. Beef, liver, shellfish and nuts provide zinc.
- After you’ve recovered from surgery, you should be able to perform most of your usual activities, the UMMC notes.
- When you’re ready to progress to a regular diet, include foods that support your immune system and promote healthy wound healing.
Related Articles
References
- MedlinePlus: Total Colectomy or Proctocolectomy: Discharge
- Cleveland Clinic: Total Abdominal Colectomy: Basic Surgical Steps
- MedlinePlus. Total abdominal colectomy. Updated September 3, 2018.
- Cleveland Clinic. Eating right and avoiding dehydration after bowel surgery. Updated Sept 3, 2010.
- Hogan BV, Peter MB, Shenoy HG, Horgan K, Hughes TA. Surgery induced immunosuppression. Surgeon. 2011;9(1):38-43. doi:10.1016/j.surge.2010.07.011
- U.S. National Library of Medicine. Medline Plus. Total Colectomy or Proctocolectomy Discharge.
Resources
Writer Bio
Anne Tourney specializes in health and nutrition topics. She is a registered nurse with experience in medical-surgical nursing, behavioral health and geriatrics. Tourney earned a Bachelor of Science in nursing from Regis University.