Causes of Itchy Skin Rashes Under the Breast
Bacteria and fungi are everywhere, but sometimes they set up shop on the skin and cause a rash. Warm, moist areas -- like under the breasts -- are more prone to these skin rashes than other areas of the body. Fungal and bacterial infections are common culprits, but skin allergies and even the chronic skin disorder psoriasis can lead to itchy skin rashes under the breasts 3. If you have a persistent rash under the breasts, see your doctor. Keeping skin clean and dry, looking out for possible allergic triggers, and seeing a dermatologist when necessary can prevent rashes from coming back.
Fungal Infections
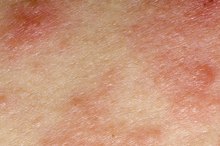
Fungal infections are a common cause of an itchy rash under the breast. A type of yeast known as Candida is the most frequent offender. Candida-related skin rashes are typically red, but white, scaly areas may form as well. Uncontrolled diabetes, antibiotic use, chronic steroid use, obesity and HIV are risk factors for Candida skin infections. Fungal skin infections tend to clear up quickly with topical antifungal creams like ketoconazole. Keeping the area dry by sprinkling antifungal powder, such as nystatin (Nystop powder), under the breasts can also help. Removing damp clothing -- especially bras -- as soon as possible and drying skin thoroughly after showering can help prevent future rashes.
- Fungal infections are a common cause of an itchy rash under the breast.
- Removing damp clothing -- especially bras -- as soon as possible and drying skin thoroughly after showering can help prevent future rashes.
Bacterial Infection
Home Remedies for a Rash Under the Breast
Learn More
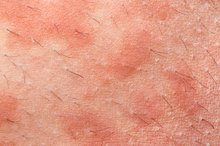
Itchy rashes under the breast can be caused by bacteria, especially Staphylococcus and Streptococcus bacteria. As with Candida infections, diabetes and immune system disorders are risk factors. However, minor skin trauma can allow bacteria to invade the skin and cause an infection in someone without risk factors. Bacterial skin rashes are usually bright red, may be slightly raised and are often warm to the touch. Oral antibiotics, such as dicloxacillin, amoxicillin-clavulanate (Augmentin) and clarithromycin (Biaxin), are necessary to treat rashes caused by a bacterial infection.
- Itchy rashes under the breast can be caused by bacteria, especially Staphylococcus and Streptococcus bacteria.
- However, minor skin trauma can allow bacteria to invade the skin and cause an infection in someone without risk factors.
Allergic Dermatitis
Skin allergies can also lead to rashes under the breast. A skin rash due to an allergy is known as allergic dermatitis. Allergic dermatitis is commonly red and very itchy. People with a history of asthma, seasonal allergies or eczema -- dry, flaky, inflamed skin -- on other parts of the body are at increased risk for allergic dermatitis. Allergic triggers vary from person to person, but laundry detergents, perfumes and lotions are often to blame. Topical steroids, like hydrocortisone (Cortizone 10, Cortaid) are the treatment of choice. Long-term use of topical steroids should generally be avoided since they can lead to skin changes and promote the overgrowth of Candida and other fungi.
- Skin allergies can also lead to rashes under the breast.
- A skin rash due to an allergy is known as allergic dermatitis.
Psoriasis
Causes of an Inner Groin Rash
Learn More
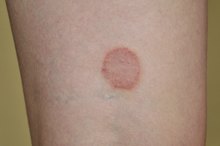
Psoriasis is a chronic skin disorder that causes patches of itchy, red, scaly skin. It most commonly affects the elbows and knees. A subtype of psoriasis known as inverse psoriasis, however, develops in skin folds under the arms, in the groin and under the breasts. Authors of a March 2013 article in the "Journal of the American Board of Family Medicine" note that inverse psoriasis is often mistaken for a Candida infection 4. However, psoriasis does not get better with antifungal creams. Topical steroids can be effective, but other psoriasis medications may be needed to prevent flareups.
Reviewed by: Tina M. St. John, M.D.
- Psoriasis is a chronic skin disorder that causes patches of itchy, red, scaly skin.
Related Articles
References
- ISRN Preventive Medicine: Candida Infections and Their Prevention
- Allergy, Asthma and Clinical Immunology: Atopic Dermatitis
- American Family Physician: Common Bacterial Skin Infections
- Journal of the American Board of Family Medicine: Resistant "Candidal Intertrigo" -- Could Inverse Psoriasis Be the True Culprit?
- Mease PJ, Armstrong AW. Managing patients with psoriatic disease: the diagnosis and pharmacologic treatment of psoriatic arthritis in patients with psoriasis. Drugs. 2014;74(4):423-41. doi:10.1007/s40265-014-0191-y.
- National Psoriasis Foundation. About Psoriatic Arthritis.
- American Academy of Dermatology. Psoriasis Resource Center.
- Haroon M, Kirby B, FitzGerald O. High prevalence of psoriatic arthritis in patients with severe psoriasis with suboptimal performance of screening questionnaires. Ann Rheum Dis. 2013;72(5):736-40. doi:10.1136/annrheumdis-2012-201706.
- Liu JT, Yeh HM, Liu SY, et al. Psoriatic arthritis: Epidemiology, diagnosis, and treatment. World J Orthop. 2014;5(4):537–543. doi:10.5312/wjo.v5.i4.537.
- National Psoriasis Foundation. Could You Have Psoriatic Arthritis? Know the Signs.
- Psoriasis Speaks. What is Psoriasis?
- Arias-Santiago, S.; Espinera-Carmona, M.; and Aneiros-Fernandez, J. The Koebner phenomenon: psoriasis in tattoos. CMAJ. 2013 Apr 16;185(7):585. doi:10.1503/cmaj.111299
- Guglielmetti, A.; Conlledo, R.; Bedoya, J. et al. Inverse Psoriasis Involving Genital Skin Folds: Successful Therapy with Dapsone. Dermatol Ther (Heidelb). 2012 Dec;2(1):15. doi:10.1007/s13555-012-0015-5
Resources
Writer Bio
Niya Jones is a physician and medical writer. She is board-certified in internal medicine and has a special interest in cardiology, particularly as it relates to health care disparities and women's health. She received her medical degree and Masters of public health from Yale University.