For centuries, people have expressed themselves through body piercings. Piercings that were once considered tribal or barbaric are now part of mainstream culture. Nipple piercing, for one, has grown tremendously in popularity among men and women, young and old, but they carry with them the risk of hypertrophic scars. Understand this risk prior to obtaining a nipple piercing.
History of Nipple Piercing
According to the experts at Painful Pleasures, a body jewelry Web site, nipple piercing can be traced back as far as the Roman Centurions. It wasn’t until the late 1890s, however, that piercing the nipples truly came into fashion. Wealthy women in Paris and London had both nipples pierced with Bosom Rings that enlarged the nipples, made them more sensitive, and provided a constant stimulation and increased sexual stimulation.
Post-Piercing Nipple Development
What Is the Bump on My Nipple Piercing?
Learn More
Elayne Angel, author of "The Piercing Bible: The Definitive Guide to Safe Body Piercing," explains that pierced nipples are prone to development, which is a semi-permanent or permanent change in the shape, dimensions, and texture of the nipple and areola. The nipple grows in response to the piercing and jewelry stimulation. This development is most common in male nipples and young, underdeveloped female nipples, and overall change can be quite dramatic. Development should not be confused with the temporary swelling other body parts may experience after piercing.
When placed in the natural creases of the body, nipple piercing results in development that is well-formed and attractive. If the piercing is made in the wrong spot, the tissue can develop an awkward, unattractive appearance that may remain even after jewelry is removed.
- Elayne Angel, author of "The Piercing Bible: The Definitive Guide to Safe Body Piercing," explains that pierced nipples are prone to development, which is a semi-permanent or permanent change in the shape, dimensions, and texture of the nipple and areola.
Defining Hypertrophic Scars
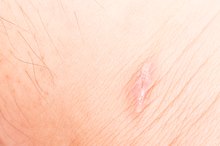
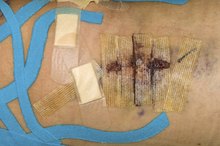
The hypertrophic scar is a variation of normal wound healing. Hypertrophic scars are raised fibrous lesions that result from trauma to the skin, such as piercings. While hypertrophic scars are generally of cosmetic concern, their presence can result in disfigurement and a loss of function. Furthermore, hypertrophic scars can be tender or painful.
- The hypertrophic scar is a variation of normal wound healing.
- Hypertrophic scars are raised fibrous lesions that result from trauma to the skin, such as piercings.
Hypertrophic Scarring Risk Factors
Scars From Belly Rings
Learn More
Dr. D.J. Verret is the founder of Innovative Facial Plastic Surgery and Wellness Center in Plano, Texas. Verret explains that nipples are no more prone than other areas of the body to hypertrophic scars, but certain populations are more at risk.
Hypertrophic scarring can occur in any person, but individuals who are African-American, Asian, or Hispanic, or those with a previous history of abnormal scarring, have the highest risk of developing a hypertrophic scar from nipple piercing 1.
- D.J.
- Verret is the founder of Innovative Facial Plastic Surgery and Wellness Center in Plano, Texas.
- Verret explains that nipples are no more prone than other areas of the body to hypertrophic scars, but certain populations are more at risk.
Preventing and Repairing Hypertrophic Scars Caused by Nipple Piercing
According to Verret, the development of hypertrophic scars is not completely understood. For this reason, it’s difficult to determine whether the piercing, the jewelry, or both is the cause.
Verret explains that any injury to the skin—whether whether surgical, intentional, or accidental—causes wound healing, which can go awry and result in a hypertrophic scar.
Hypertrophic scars may also result from the presence of a foreign material, such as nipple jewelry, but removal of the jewelry does not affect the growth or regression of the hypertrophic scar. The jewelry must be removed, however, to remove the scar with surgical treatment and closure of the piercing.
Hypertrophic scars will grow only in the area of the original scar and will often improve over time. According to Verret, injecting the scar with steroids can help.
- According to Verret, the development of hypertrophic scars is not completely understood.
- Verret explains that any injury to the skin—whether whether surgical, intentional, or accidental—causes wound healing, which can go awry and result in a hypertrophic scar.
Re-Piercing after Hypertrophic Scar Removal
After the hypertrophic scar has been removed, the nipple can be re-pierced; however, the risk of development of another abnormal scar is high.
Related Articles
References
- PainfulPleasures.com: Body Piercing History
- Jacobs VR, Golombeck K, Jonat W, Kiechle M. Mastitis nonpuerperalis after nipple piercing: time to act. Int J Fertil Womens Med. 2003;48(5):226-31.
- Gardner SE, Frantz RA, Troia C, et al. A tool to assess clinical signs and symptoms of localized infection in chronic wounds: development and reliability. Ostomy Wound Manage. 2001;47(1):40-7.
- World Health Organization. Hepatitis B. Published July 18, 2019.
- Leibman AJ, Misra M, Castaldi M. Breast abscess after nipple piercing: sonographic findings with clinical correlation. J Ultrasound Med. 2011;30(9):1303-8. doi:10.7863/jum.2011.30.9.1303
- Lee B, Vangipuram R, Petersen E, Tyring SK. Complications associated with intimate body piercings. Dermatol Online J. 2018;24(7).
- Breuner CC, Levine DA; Committee on Adolescence. Adolescent and Young Adult Tattooing, Piercing, and Scarification. Pediatrics. 2017 Oct;140(4). pii: e20163494. doi: 10.1542/peds.2017-1962. Epub 2017 Sep 18.
- Castillo M, Sanjuán A, Pérez N, Zanón G, Bons N, Vilanova M, et al. Fibrous Histiocytoma-like Spindle-Cell Proliferation in the Nipple After Body-Piercing. Int J Surg Pathol. 2006 Jan;14(1):89-93.
- Lee B, Vangipuram R, Petersen E, Tyring SK. Complications associated with intimate body piercings. Dermatol Online J. 2018 Jul 15;24(7). pii: 13030/qt5gp333zr.
- Robyn Roche-Paull, RNC-MNN, BSN, IBCLC. Nipple Piercings. La Leche League. https://www.llli.org/breastfeeding-info/nipple-piercings/
Writer Bio
Mary Fetzer is a freelance writer, blogger and marketing consultant. She has a marketing degree from Penn State University and 15 years of international business experience. Fetzer covers a variety of subjects, including relationships, pregnancy, parenting, health, finance, real estate, entertainment news, baby names and education. Her marketing expertise includes marketing research and competitor analysis.