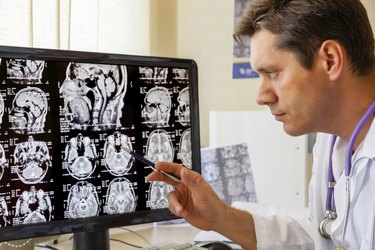
Schizophrenia is a complex brain disorder that affects a person's ability to perceive reality. Common symptoms include false beliefs; seeing objects that are not present; hearing voices; disorganized thoughts and speech; and emotional detachment or instability. The National Institute of Mental Health reports that approximately 1 percent of the U.S. population has schizophrenia, with men and women affected equally. The major brain regions affected include the prefrontal cortex, the basal ganglia and the limbic system.
Prefrontal Cortex
Video of the Day
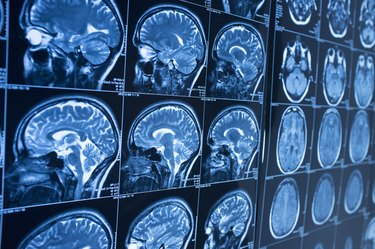
The prefrontal cortex is the brain region directly behind the forehead. This brain area is mainly responsible for complex tasks known as executive functions, including decision-making, strategizing and adjusting behaviors according to social cues or past experience. Improper function of the prefrontal cortex results in loss of these capabilities and the characteristic disordered thinking of schizophrenia. Impaired function of the prefontal cortex in people with schizophrenia may be related to the excessive release of the brain chemical dopamine.
Video of the Day
Basal Ganglia

The variety of symptoms seen with schizophrenia may be a result of how highly interconnected the brain is. For example, the prefrontal cortex is connected to another brain area affected in schizophrenia called the basal ganglia. This region is known for producing dopamine and regulates coordinated movement, motivation and the reward pathway. This complex pathway reinforces patterns of behavior that make a person feel good. A July 2013 study report published in "Biological Psychiatry" noted that brain imaging studies demonstrate increased activity in the basal ganglia and decreased connectivity between this region and the prefrontal cortex in people with schizophrenia.
Limbic System
The limbic system consists of brain structures that are primarily responsible for learning and memory as well as processing emotion. Similar to the decreased connections between the prefrontal cortex and the basal ganglia, a February 2015 study report published in "European Psychiatry" found altered connectivity between parts of the limbic system and the prefrontal cortex in people with schizophrenia. Moreover, abnormal brain chemistry of the limbic system has also been implicated in contributing to schizophrenia.
Reduced Brain Volume
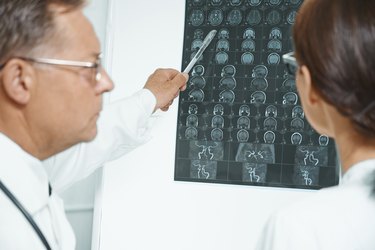
The reduced level of connections among these brain areas and alterations in brain chemicals are key findings that may explain the symptoms and abnormal behavior seen in people with schizophrenia. Evidence also points to reduced brain volume, however. A study published in October 2012 in the "Schizophrenia Bulletin" reported that people with schizophrenia have slightly smaller brains compared to those without the disorder. The authors further noted that this finding occurs early in the disease and tends to become more pronounced over time.
- Adrian Preda, MD, professor of clinical psychiatry at the University of California Irvine in Orange.
- eNeuro: “Synaptic Wiring of Corticostriatal Circuits in Basal Ganglia: Insights into the Pathogenesis of Neuropsychiatric Disorders.”
- Psychiatry Research: “Amygdala volume is reduced in early course schizophrenia.”
- Neuroanatomy: “Prefrontal Cortex.”
- Neuroanatomy: “Hippocampus.”
- F1000Research: “Recent advances in understanding the role of the basal ganglia.”
- National Institutes of Health: “New Findings Reveal Surprising Role of the Cerebellum in Reward and Social Behaviors.”
Is this an emergency? If you are experiencing serious medical symptoms, please see the National Library of Medicine’s list of signs you need emergency medical attention or call 911.